TC and PC may also be paid separately using a modifier (TC for Technical Component and − 26 for Professional Component) appended to the CPT code. In the clinical laboratory, some services have a defined PC, such as: 86077 Blood bank physician services; difficult cross match and/or evaluation of irregular antibody(s), interpretation, and written report .
RVUs are more complex than we have stated so far. In fact, the RVU for the PC is composed of three components: actual physician work, practice expense, and malpractice.
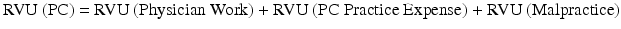
Similarly, TC RVUs are calculated by summing RVU subcomponents for TC practice expense and malpractice :
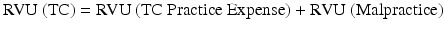
So how might one calculate an individual payment for a service using RVUs? The CMS website provides a fee schedule search function that also yields RVU values (http://cms.gov/apps/physician-fee-schedule/search/search-criteria.aspx).
The CF is also available on the CMS website and as of September 2015 is US $35.9335.
So we can calculate for the 2015 National Average Medicare Physician Fee Schedule:
88305 PC = [RVU (Work) + RVU (PC Practice Expense) + RVU (Malpractice)] × CF =
[0.75 + 0.33 + 0.01] × US$35.9335 = US $ 39.1675 = $ 36.17
88305 TC = [RVU (TC Practice Expense) + RVU (Malpractice)] × CF
= [0.94 + 0.01] × US$35.9335 = US $ 34.1368 = $ 34.14
88305 Global = US$39.1675 + US $ 34.1368 = US $ 73.3043 = US $ 73.30
There is yet another complexity before we actually collect a dime. Geographic Practice Cost Indices (GPCIs) are used to adjust individual RVU components to account for geographic variations in costs to provide services. For example, it is less expensive to run a practice in, say, Oklahoma City than many other places in the country. As such, PC RVUs in Oklahoma City are adjusted downward in 2015 for RVU (practice expense) and RVU (malpractice) by factors of 0.872 and 0.845, respectively .
For the PC

2015 Oklahoma Medicare Fee Schedule
![$$\begin{aligned} 88305\rm{PC} & = [(0.75 \times 1.000) + (0.33 \times 0.872) + (0.01 \times 0.845)] \times \rm{ US}\$ 35.9335 \\ & = \rm US\$ 37.59 \end{aligned}$$](/wp-content/uploads/2016/10/A315358_1_En_1_Chapter_Eque.gif)
(National Average 88305 PC = US$39.17)
So, if you provide Part B services, just submit the appropriate and complete CPT codes to Medicare with the proper documentation, and you can calculate the payment you can receive using data from the CMS.gov website .
Key Concept
CPT codes determine payment via linkage to RVUs for both technical and professional component work.
An additional point to be aware of is that Medicare adjusts payments to physicians through its Physician Quality Reporting System (PQRS) which entails specific reporting in select cases that, as a good lab, you are probably already doing coupled with specific codes to report that you did the right thing. We encourage you to look more closely at the PQRS process particularly if you have significant payments coming from Medicare. Initially, there were modest percentage increases in all of an individual’s Medicare payments for correctly reporting an appropriate percentage and number of eligible cases . For 2014 and beyond, there are increasing penalties for nonparticipation/non-reporting. For 2015, there are eight measures for pathologists, the five original involving breast cancer resections, colorectal cancer resections, radical prostatectomy cases, biopsies with Barrett’s esophagus, and cases with Her-2/Neu immunohistochemical stain reporting, and three new for 2015 measures involving lung cancer and melanoma reporting. Failure to report in 2014 resulted in a 2 % penalty applied to all Medicare Part B payments to be made in 2016. Participation in 2015 PQRS will impact the 2017 PQRS adjustments and 2017 value-based modifier (CAP Today November 2014).
Medicaid is a joint federal and state program using basic federal benefits but with significant state-to-state variability. Individual state programs set their own payment rate structures that are CPT-code-based but which usually pay less than Medicare . Medicaid is subordinate to Medicare for patients who have both benefits .
Insurance and managed care cover a range of products and payors. Historically, indemnity insurance had limited or no utilization controls, less focus on preventative care, and higher patient premiums than for other types of insurance, corresponding to a higher degree of patient autonomy or choice, and hence utilization. The term managed care covers a range of products and payment systems but typically involves targeted contracting and utilization controls. Payments from insurance and managed care can range from a percentage of billed charges to a negotiated (or take-it-or-leave-it) fee schedule, often some percentage of Medicare payments, to some form of “capitation” in which providers receive a set sum per month for all services provided to a patient or group of patients (“per-member-per-month” agreements). For patients who do not have any insurance or who are self-pay, the individuals are billed, and collections are quite variable from individual to individual. Usually, collections from this subset of patients are relatively limited .
Recent Trends and Changes
More recently, we see a growing call to move away from fee-for-service coupled with a trend to link payment rates to process and outcome measures. There is often a downside possibility for providers as well as upside potential (shared savings). In an attempt to reduce health-care costs, both federal and private insurers are experimenting with bundled payments and accountable care organizations (ACOs) . Bundled payments use a larger single payment for either a range of services or a range of providers in an effort to reduce total payments. Providers may thereby be encouraged to reduce services or negotiate among themselves to achieve the savings. ACOs are groups of providers, sometimes including hospitals, that organize to become “accountable” for managing care across a population or chronic disease to encourage providers to better coordinate care in return for potential shared savings. For these new and growing models, it is important for the pathologist to be aware of what is happening in their service area and be proactive where possible by improving care pathways, test utilization, information management, and overall care coordination.
In April 2015, physicians rightly cheered the repeal of the sustainable growth rate (SGR) formula which was designed to limit the growth in Medicare payments to the growth in gross domestic product. Enacted by legislation in 1997, the SGR would have led to dramatic reductions in payments for Medicare services, but the cuts were routinely blocked by Congress with a series of legislative actions that blocked full implementation of SGR such that the indicated cuts in Medicare payments to physicians would have exceeded 20 %. In fact, at the time of SGR repeal, a scheduled decrease of 21.2 % in physician payments for Medicare patients hung over physicians as a distinct threat. While it is always treacherous to speculate on political wranglings, the SGR “fix” was a challenge because, on the one hand, repeal of the SGR has significant costs in federal dollars over a 10 year period in a time of substantial federal deficits, while on the other hand, a one-time cut in Medicare payments of the magnitude indicated (greater than 20 %) would probably have disrupted provision of Medicare services creating access issues for America’s seniors and creating undue hardship for some medical practices.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


