Eating Disorders
KEY CONCEPTS
![]() The identification and acceptance of eating disorders as a psychiatric illness is increasingly common. They remain difficult to treat as effectiveness trials are limited, and patients are inherently resistant to accepting treatment.
The identification and acceptance of eating disorders as a psychiatric illness is increasingly common. They remain difficult to treat as effectiveness trials are limited, and patients are inherently resistant to accepting treatment.
![]() Eating disorder not otherwise specified is currently the most commonly diagnosed form of eating disorder; however, proposed changes to the diagnostic criteria in the fifth edition of the Diagnostic and Statistical Manual of Mental Disorders would separate binge eating disorder as a stand-alone diagnosis.
Eating disorder not otherwise specified is currently the most commonly diagnosed form of eating disorder; however, proposed changes to the diagnostic criteria in the fifth edition of the Diagnostic and Statistical Manual of Mental Disorders would separate binge eating disorder as a stand-alone diagnosis.
![]() Despite strong genetic associations for the development of eating disorders as established in monozygotic and dizygotic twin studies, a clear association with a specific genetic link mutation has not been identified.
Despite strong genetic associations for the development of eating disorders as established in monozygotic and dizygotic twin studies, a clear association with a specific genetic link mutation has not been identified.
![]() Shifting between eating disorder diagnostic categories is possible, especially when symptom remission is not achieved with treatment.
Shifting between eating disorder diagnostic categories is possible, especially when symptom remission is not achieved with treatment.
![]() Psychiatric comorbidities are common with all forms of eating disorders, and the differential diagnosis should generally include evaluation for depression, schizophrenia, generalized anxiety, and obsessive–compulsive and personality disorders.
Psychiatric comorbidities are common with all forms of eating disorders, and the differential diagnosis should generally include evaluation for depression, schizophrenia, generalized anxiety, and obsessive–compulsive and personality disorders.
![]() During the process of caloric restoration, calories must be gradually introduced to prevent the potentially fatal complication known as refeeding syndrome.
During the process of caloric restoration, calories must be gradually introduced to prevent the potentially fatal complication known as refeeding syndrome.
![]() Mortality resulting from suicide in eating disorders is not uncommon, and clinicians must monitor closely for suicidality and educate appropriately as they would during the treatment of patients with major depressive disorder with antidepressant therapy.
Mortality resulting from suicide in eating disorders is not uncommon, and clinicians must monitor closely for suicidality and educate appropriately as they would during the treatment of patients with major depressive disorder with antidepressant therapy.
![]() The current preferred treatment approach for anorexia nervosa includes a minimum of 6 months of psychotherapy, preferably cognitive behavioral therapy.
The current preferred treatment approach for anorexia nervosa includes a minimum of 6 months of psychotherapy, preferably cognitive behavioral therapy.
![]() Data supporting the use of medication in anorexia nervosa are largely inconclusive. Primary limitations are small sample sizes and a bias in clinical trials because more highly motivated patients participate in studies.
Data supporting the use of medication in anorexia nervosa are largely inconclusive. Primary limitations are small sample sizes and a bias in clinical trials because more highly motivated patients participate in studies.
Eating disorders are widely accepted as serious mental illnesses. The spectrum of eating disorders encompasses several complex diseases, sharing the pathologic feature of overevaluation of body shape and weight. Eating disorders arise from the interaction between environmental, societal, developmental, psychosocial, genetic, and biologic factors. It is estimated that 5 to 10 million women and 1 million men in the United States alone have an eating disorder. The urbanization of society, social pressure, and obsession with perfection and being thin have led to an increasing prevalence of eating disorders, with the peak onset being between 16 and 20 years of age.1–4 Anorexia nervosa (AN), bulimia nervosa (BN), and eating disorders not otherwise specified (EDNOS) are the primary disorders that have been identified.5
![]() Despite an improved understanding of these cognitively and emotionally disabling and potentially fatal disorders, management remains difficult. Pharmacologic intervention is a small part of a comprehensive plan that emphasizes cognitive behavioral therapy (CBT) and psychotherapy.
Despite an improved understanding of these cognitively and emotionally disabling and potentially fatal disorders, management remains difficult. Pharmacologic intervention is a small part of a comprehensive plan that emphasizes cognitive behavioral therapy (CBT) and psychotherapy.
EPIDEMIOLOGY
Anorexia Nervosa
AN occurs predominantly in girls and young women (90%) and usually presents in late adolescence (median onset 17 years of age), with new cases rarely diagnosed after age 40. The estimated prevalence of the disorder in the general population is 0.9% of females and 0.3% of males.6 Longitudinal management of AN is difficult, as patients are often resistant to weight restoration plans. Rates of relapse requiring hospitalization within 1 year exceed 30%, and crude mortality rates are estimated at 4%.7,8
The promotion of the virtues of being thin is also a potentially negative environmental factor. Many websites, for example, inappropriately promote healthy lifestyle aspects of anorexia and being thin as a means of being in control, successful, and coping with life’s pressures.9
Bulimia Nervosa
BN also occurs predominantly in girls and young women (90%) and usually presents in adolescence or early adult life.6 Between 1% and 4.6% of adolescent and young adult females meet the diagnostic criteria for BN, with lifetime prevalence estimates of 1.5% of females and 0.5% of men.3,5,6,10,11
Eating Disorder Not Otherwise Specified
EDNOS is also described in the American Psychiatric Association’s Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition, Text Revision (DSM-IV-TR).3,5 Originally designed to capture eating disorder cases that did not meet diagnostic criteria of AN or BN, it has instead developed into a diagnosis of indifference. ![]() The overall prevalence of EDNOS is estimated at 3.5% among women and 2% in men, the highest prevalence of the eating disorders.6 An estimated 50% of patients with an eating disorder admitted to tertiary care settings are believed to have this condition.12 These individuals present with symptoms characteristic of eating disorders but do not meet specific diagnostic criteria. Two examples of EDNOS are night eating syndrome (NES) and binge eating disorder (BED).
The overall prevalence of EDNOS is estimated at 3.5% among women and 2% in men, the highest prevalence of the eating disorders.6 An estimated 50% of patients with an eating disorder admitted to tertiary care settings are believed to have this condition.12 These individuals present with symptoms characteristic of eating disorders but do not meet specific diagnostic criteria. Two examples of EDNOS are night eating syndrome (NES) and binge eating disorder (BED).
NES is common in obesity clinic populations, often accompanied by depressive symptoms. The syndrome is defined by early morning anorexia, hyperphagia in the evening, nighttime insomnia, and subsequent early morning awakening.5,13 NES affects an estimated 1.5% of the general population and 8.9% to 27% of patients in obesity clinics.14–16 Patients with NES are reported to benefit from antidepressant therapy, most notably sertraline 50 to 200 mg daily.13
The diagnostic criteria for BED describe recurrent episodes of binge eating without compensatory behaviors (e.g., purging, excessive exercise, or fasting). BED typically presents later in life (older than 40 years of age), and approximately one fourth of BED patients are male.12,17 CBT and interpersonal psychotherapy are the preferred treatments, although antidepressant therapy has also demonstrated limited benefits.17
ETIOLOGY AND PATHOPHYSIOLOGY
While the exact etiology of eating disorders is not known, it is most likely a combination of genetic, biologic, developmental, and environmental factors. The biologic basis for eating disorders is difficult to delineate because it is unclear if the biologic changes are caused by or are a result of the aberrant eating behavior.
Abnormalities of the hypothalamic–pituitary–gonadal, hypothalamic–pituitary–adrenal, and hypothalamic–pituitary–thyroid axes are described as potential causes of AN. Amenorrhea is found in the majority of females with anorexia, providing support for the association with gonadotropin.11
Serotonin, norepinephrine, and dopamine have been studied extensively with well-described roles in controlling eating behaviors, with more emphasis placed on the role of serotonin. Complicating the study of these abnormalities is that their dysfunction is thought to be secondary to weight loss. There is evidence suggesting serotonin and dopamine function remain abnormal after weight restoration.18,19 Another molecular genetic target of study is brain-derived neurotrophic factor (BDNF), which is also being studied in disease states such as depression.20
![]() There are strong genetic influences in AN and likely associations in both BN and BED. In addition, there is a high degree of premorbid anxiety and obsessive tendencies, which are also symptoms of disorders with suspected genetic associations. Twin studies have shown concordance of ∼55% and 35% in monozygotic twins and 5% and 30% in dizygotic twins for AN and BN, respectively.
There are strong genetic influences in AN and likely associations in both BN and BED. In addition, there is a high degree of premorbid anxiety and obsessive tendencies, which are also symptoms of disorders with suspected genetic associations. Twin studies have shown concordance of ∼55% and 35% in monozygotic twins and 5% and 30% in dizygotic twins for AN and BN, respectively.
One of the most common areas of research has centered on the roles of serotonin, dopamine, and norepinephrine. Serotonin is the most commonly studied neurotransmitter in patients with eating disorders, but its study is complicated by the fact that it is affected by other factors including sex hormones. In addition, reduced dietary intake of food leads to reduced levels of tryptophan, which is required for the development of serotonin.18–20 Serotonin activity is abnormally high in patients recovered from AN. In addition, serotonin 2A receptors are reduced after recovery, while dopamine receptors are increased.18–20
Genetic-based linkage studies have examined multiple single nucleotide peptides to identify predictors for developing AN, which may subsequently help identify appropriate pharmacologic treatments. Studies to date have identified possible associations with chromosomes #1, #2, #3, #4, and #13; however, there are no consistent findings to date, and studies are limited by low sample size.18,21,22 Genetic mutation studies have focused on polymorphisms of the serotonin 2A receptor.17 One acquired hereditary abnormality being studied is the presence of low-function alleles associated with the serotonin transporter (5-HTTLPR) and serotonin 2A receptor gene (–1438G/A), with findings suggesting an association with poor treatment response.23 Recent work has also associated estrogen receptor I gene (ESRI) with the restrictive form of AN.24
Emphasis is also placed on environmental factors such as social stress and psychological and developmental issues related to dysfunctional family relationships triggering abnormal eating behavior.3,11,12,25 Athletes are at risk for eating disorders, especially female gymnasts, ballet dancers, figure skaters, distance runners, swimmers, male wrestlers, and body builders.26
DIAGNOSTIC CRITERIA AND CLINICAL PRESENTATION
AN and BN occur together in ∼30% to 64% of patients with eating disorders, and they may not be distinct diagnostic entities, but rather a continuum of symptoms. Thus, careful medical and psychiatric assessment at baseline is essential.27–30 ![]() Patients who initially present with either AN or BN may alternate from one to the other, especially in cases where remission is not achieved. Figure 47-1 demonstrates similar and unique features of both disorders.
Patients who initially present with either AN or BN may alternate from one to the other, especially in cases where remission is not achieved. Figure 47-1 demonstrates similar and unique features of both disorders.
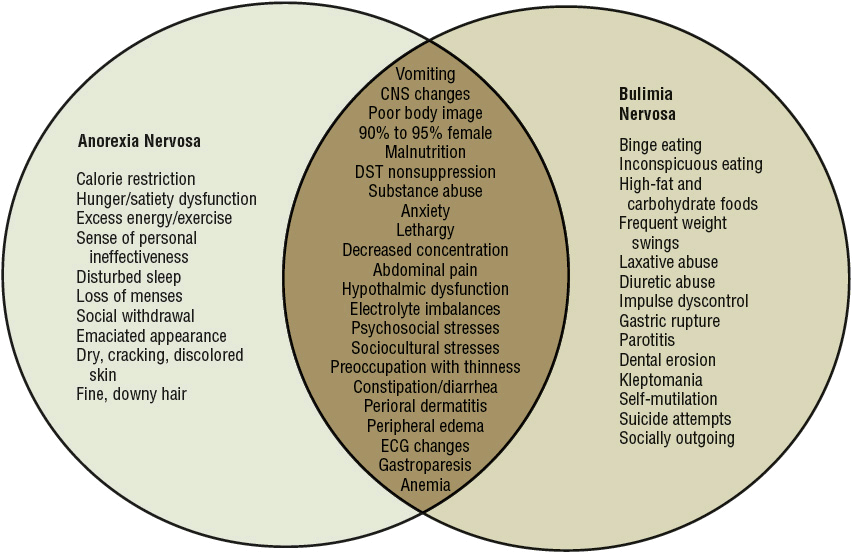
FIGURE 47-1 Signs and symptoms of anorexia nervosa and bulimia nervosa. (DST, dexamethasone suppression test; ECG, electrocardiogram.)
The use of purging methods is not limited to BN. Self-induced vomiting is the most common form of purging behavior.31 Laxative abuse is another form of purging common in both AN and BN, used by an estimated 3% to 70% of patients.31–33 Although ineffective as a weight-loss strategy, laxative abuse is often used in combination with other behaviors, including exercise, diuretics, enemas, and saunas. Within the diagnostic framework of AN, laxative abuse is most common in those identified with the purging subtype.31 Psychiatric symptoms of depression, anxiety, and borderline personality disorder are also reported in those who abuse laxatives.31–33
Depression, schizophrenia, obsessive–compulsive disorder (OCD), and conversion disorders should be included in the differential diagnosis of AN and BN, as eating abnormalities can be a component of these illnesses. The salient differences are the overriding drive for thinness, disturbed body image, increased energy directed at losing weight, and binge eating episodes that are relatively specific for eating disorders. Most patients with eating disorders experience relief of psychiatric symptoms on refeeding.12
Anorexia Nervosa
The presentation of AN includes a recent period of weight loss as well as associated behaviors to promote this such as vomiting, limiting food intake, and excessive exercise. Current diagnostic criteria for AN include the refusal to maintain a minimal normal body weight, failure to make expected weight gains, intense fear and obsession about weight gain or being “fat,” distorted body image, and amenorrhea for at least three consecutive cycles.5 Patients typically lack an appreciation for the degree of weight loss experienced or are preoccupied with the idea that a part of their body is too large, despite evidence to the contrary. The DSM-IV-TR further classifies AN as restricting type (restricting food intake with no binge eating or purging behavior) or binge eating/purging type, in which patients regularly participate in bingeing or purging.5 The anorexic patient has difficulty sensing when he or she is full (satiety) and commonly complains of feeling bloated after eating. Patients also describe not feeling in control of various aspects of their life, particularly caloric intake. Comorbid psychiatric conditions, such as major depression, are frequent but should initially be considered secondary to starvation and not a true mood disorder.
The fifth edition of the Diagnostic and Statistical Manual of Mental Disorders (DSM-V) is scheduled for release in 2013. A DSM-V work group is recommending a number of changes to the diagnosis of AN.34 These include the following: elimination of descriptive examples for body weight maintenance, adding behavior as a symptom for failing to gain weight, removal of amenorrhea as a diagnostic component, and limiting the subclassifications of AN to symptoms exhibited in the prior 3 months.22,34,35
![]() Psychiatric comorbidity is common, as up to 75% of patients have a primary mood disorder, and there is also an association with personality disorders and anxiety disorders, such as social phobia and OCD.36 The lifetime prevalence of OCD in patients with AN is reported to be as high as 40%; the lifetime prevalence in the general population is 2.5%.36–38 The impact that psychiatric comorbidity has on treatment outcomes of AN is unknown, but it is important to understand that deprivation of food may contribute to both mood and cognitive fluctuations.
Psychiatric comorbidity is common, as up to 75% of patients have a primary mood disorder, and there is also an association with personality disorders and anxiety disorders, such as social phobia and OCD.36 The lifetime prevalence of OCD in patients with AN is reported to be as high as 40%; the lifetime prevalence in the general population is 2.5%.36–38 The impact that psychiatric comorbidity has on treatment outcomes of AN is unknown, but it is important to understand that deprivation of food may contribute to both mood and cognitive fluctuations.
Bulimia Nervosa
The core feature of BN is recurrent episodes of binge eating (an excessive intake of calorie-laden food over a short period of time). Persons with BN are overly sensitive about their weight and have a distorted body image. Most have normal weight, although they might fluctuate between being underweight and overweight. Patients lack control over their eating and participate in recurrent compensatory behavior to prevent weight gain. These behaviors may include self-induced vomiting; misuse of laxatives, diuretics, enemas, or other medications; strict dieting or fasting; or excessive exercise. To meet DSM-IV-TR criteria, the binges and compensatory behaviors must occur on average at least twice weekly for 3 months.5 BN can further be differentiated by purging type (regularly engages in self-induced vomiting or the misuse of laxatives, diuretics, or enemas) or nonpurging type (uses other inappropriate compensatory behaviors, such as fasting or excessive exercise, but does not engage in purging activities).5
The DSM-V work group has proposed standardization of the frequency of symptoms for BN and BED, reducing the requirement of binges and compensatory behavior to one time per week for 3 consecutive months.34 Subclassifications of BN would be eliminated in the new edition, with BN including what was formerly recognized as the purging form. The nonpurging form would now fall under the category of BED. By broadening the criteria, the size of the population in the EDNOS category should be reduced.
CLINICAL PRESENTATION Anorexia Nervosa
CLINICAL PRESENTATION Bulimia Nervosa
Patients typically binge and vomit at least once daily. Caloric intake varies, but patients can consume between 5,000 and 20,000 cal (20,929 and 83,716 J) during a single binge. Patients tend to consume foods that are easy to ingest, do not require much chewing or preparation, and are high in carbohydrates or fat. Binge eating is typically secretive and precipitated by a stressful event, followed by postbinge remorse. Binges often last less than 2 hours but can extend to more than 8 hours. To compensate for the excessive caloric intake, many patients fast for prolonged periods, exercise compulsively, purge, or abuse laxatives.
Psychiatric comorbidity includes depression (up to 80%), poor impulse control, and substance abuse. Approximately 30% to 37% of bulimic patients have a personal history of substance abuse.39 Kleptomania and borderline and avoidant personality disorders are also frequently observed.36,40 Patients also commonly steal laxatives and comfort items, such as candies and clothes.11
Binge Eating Disorder
Patients with BED present with recurrent episodes of bingeing without the compensatory behaviors associated with AN or BN. It is estimated that 5% to 10% of patients seeking treatment for obesity have BED. Comorbid psychotic disorders are common and reported in greater than 70% of BED patients.41 Major depressive disorder and low self-esteem are common, although the self-deprecating focus on body image is less severe than in AN or BN.15,38 Diagnostic criteria require that episodes of bingeing occur at least twice weekly over a period of 6 months.5
Proposed changes in the DSM-V are to separate out BED from the EDNOS category and change the diagnostic criteria for bingeing frequency to only once weekly.22,34 In addition, what was formerly recognized as nonpurging BN would now be classified as BED.
MEDICAL COMPLICATIONS OF EATING DISORDERS
The potential medical complications of eating disorders involve multiple organ systems. The type of medical complication encountered is dependent on the type and frequency of the eating disorder behavior. Cardiac complications may occur and can include wasted cardiac muscle, orthostatic hypotension, decreased cardiac output, arrhythmia, and QTc interval prolongation.42 ![]() During caloric restoration, there is a potential risk for developing refeeding syndrome, which can progress to fatal cardiovascular collapse. This risk is reduced by the gradual versus rapid reintroduction of calories.
During caloric restoration, there is a potential risk for developing refeeding syndrome, which can progress to fatal cardiovascular collapse. This risk is reduced by the gradual versus rapid reintroduction of calories.
Metabolic (metabolic acidosis, metabolic alkalosis) and electrolyte disturbances (e.g., hypokalemia, hypomagnesemia, and hypocalcemia) and dehydration are often seen. Elevations in bicarbonate levels during periods of hypokalemia can be an indication that the patient is inducing vomiting or using dietary weight-loss medications. Non–anion-gap acidosis has also been reported with the abuse of laxative agents. Additionally, both acute and chronic renal failures have been reported.
GI, oropharyngeal, and dental complications are frequent, as are general complaints of lethargy and fatigue. Evidence of Russell’s sign may be present signified by skin lesions on the fingers used to induce vomiting.
Hormonal changes related to the hypothalamic–pituitary–gonadal axis resulting from starvation are seen. These abnormalities include effects on estradiol, the gonadotropins (e.g., luteinizing hormone, follicle-stimulating hormone, and gonadotropin-releasing hormone), thyroid function, adrenal function, and growth hormone.11,42 Specific to female athletes is the female athlete triad, defined by the development of irregular menses, osteoporosis, and disordered eating.42,43 An athlete may experience only one or two components of the triad, or all three conditions.44 Osteopenia, osteoporosis, and infertility are potential long-term complications of suppressed estrogen. The restoration of weight, specifically in AN, reverses the bone loss, although estrogen supplementation does not appear to be effective.45 In all cases, the preferred method to address these issues is the normalization of nutrition. The impact on female fertility is not well studied, although the ability to carry a pregnancy to term or to give birth to a child of average birth weight appears reduced.
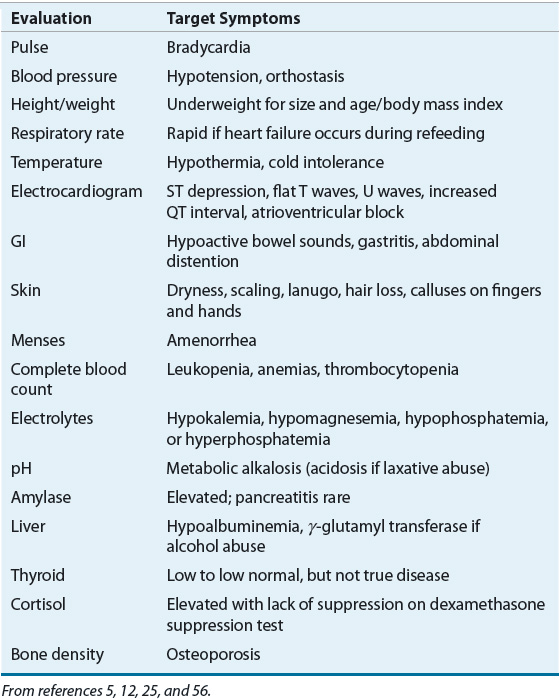
Chronic starvation can contribute to brain atrophy. Decreases in white matter and cerebrospinal fluid volumes return to normal after a healthy weight is achieved, but gray matter loss can persist.12,46,47 A thorough physical and laboratory evaluation, as described in Table 47-1, is essential to determine the severity of medical complications.5,25,48
TABLE 47-1 Physical and Laboratory Assessment of Eating Disorders