Problem 1 Difficulties with postoperative fluid balance in a 58-year-old man
A 58-year-old man is seen in the emergency department with abdominal pain and vomiting. He has been ill for 36 hours prior to this attendance, with increasingly frequent colicky abdominal pain, distension, and reduced bowel function. In the preceding 24 hours he has not passed any flatus and has vomited four times.
He had a laparotomy for a perforated appendix 5 years ago. Prior to this episode his general health had been good and his past medical history is otherwise unremarkable.
On examination he is in pain, apyrexial, and has a dry, coated tongue with loss of skin turgor. He feels thirsty and has a tachycardia of 115 beats per minute (bpm) and a (lying) blood pressure of 115/75 mmHg. On sitting, his pulse goes up to 135 bpm and his systolic blood pressure drops to 95 mmHg. Examination of his cardiovascular and respiratory systems reveals no significant abnormalities.
He is overweight, with a BMI of 30 kg/m2 (height 174 cm, weight 90 kg). His abdomen is distended, with a scar from his previous laparotomy. There are no physical signs of abdominal wall hernia. His abdomen is tense and tender on deep palpation. It is resonant, but not painful to percussion. Bowel sounds are frequent and high pitched.
Investigation 1.1 Blood results
| Haemoglobin | 165 g/L |
| White cell count | 9.6 × 109/L |
| Platelets | 350 × 109/L |
| Sodium | 149 mmol/L |
| Potassium | 3.4 mmol/L |
| Urea | 10.0 mmol/L |
| Creatinine | 0.12 mmol/L |
| Chloride | 112 mmol/L |
| Bicarbonate | 29 mmol/L |
| Glucose | 4.4 mmol/L |
| Bilirubin | 19 µmol/L |
| Total protein | 65 g/L |
| Globulins | 27 g/L |
| Albumin | 38 g/L |
| ALT | 25 U/L |
| AST | 39 U/L |
| ALP | 74 U/L |
| GGT | 17 U/L |
| LDH | 110 U/L |
| Amylase | 65 U/L |
| Calcium | 2.16 mmol/L |
| Phosphate | 1.15 mmol/L |
| Uric acid | 0.21 mmol/L |
| Cholesterol | 3.6 mmol/L |
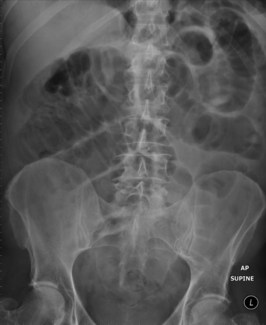
His abdominal X-ray is shown in Figure 1.1.
Conservative management has not been successful and an emergency operation is arranged.
Investigation 1.2 Fluid balance chart on admission
| Fluid Input | |
| IV fluids | 4200 mL |
| Fluid Output | |
| Urine total | 400 mL |
| Urine last 4 hours | 22/16/12/0 mL |
| Nasogastric tube | 700 mL |
| Wound drain | 200 mL |
Investigation 1.3 Fluid balance 24 hours later
| Fluid Input | |
| IV fluids | 3700 mL |
| Fluid Output | |
| Urine total | 800 mL |
| Urine last 4 hours | 15/13/9/8 mL |
| Nasogastric tube | 2800 mL |
| Wound drain | 400 mL |
The early morning electrolytes are as follows:
Investigation 1.4 Electrolytes
| Sodium | 138 mmol/L |
| Potassium | 2.7 mmol/L |
| Chloride | 102 mmol/L |
| Bicarbonate | 29 mmol/L |
| Urea | 7.0 mmol/L |
| Creatinine | 0.08 mmol/L |
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree