Bundled code
Exceptions
Uterus with fallopian tubes and ovaries
88309 (uterine tumor) or 88307 (nonneoplastic)
Ovary contains possible tumor
Mastectomy with regional lymph nodes
88309
Lymph node is designated as “sentinel” or otherwise indicated by surgeon to need separate attention
Larynx with regional nodes
88309
Surgeon requests evaluation of multiple lymph nodes by level
There are also codes for ancillary studies such as special stains and immunohistochemical stains that might be performed on a surgical pathology specimen which we will learn about later.
One of the most active areas of coding for a pathologist will be in surgical pathology . The basic codes range from 88300 gross-only code to the 88309 level VI gross and microscopic examination code which is used for the most complex specimens. We refer you to the CPT coding manuals for what each code covers because in surgical pathology we have a relatively limited number of codes to cover many different kinds of specimens. For instance, any gross-only specimen will be coded 88300. For code 88305, the AMA CPT coding manual provides a long list of covered specimens which is partially shown below. Similar lists exist for 88302, 88304, 88307, and 88309. The lists are fairly comprehensive, but if you cannot find a particular specimen type listed, the AMA instructs that you assign the code based on equivalent physician work; for example, an excisional Loop Electrocautery Excision Procedure (LEEP) cervical specimen with examination of surgical margins is commonly equated to other specimens in CPT category 88307.
For common code 88305:
Abortion—spontaneous/missed
Artery, biopsy
Bone marrow, biopsy
Bone exostosis
Brain/meninges, other than for tumor resection
Breast biopsy, not requiring microscopic evaluation of surgical margins
Breast, reduction mammoplasty
Bronchus, biopsy
Cell block, any source
Cervix, biopsy
Colon, biopsy
Duodenum, biopsy
+ 54 others
Let us take a moment for a few examples: Billing for our 88305 colon biopsy example—if you had five separately labeled colon biopsies, you would code 88305 × 5. If you had three separately labeled colon biopsies, a stomach biopsy, and an esophageal biopsy, once again, the code would be 88305 × 5 to account for the five separately identified specimens.
Skin Specimens
For skin specimens, the codes are
88300
Surgical pathology, gross examination only
88302
Skin, plastic repair
88304
Skin, cyst/tag/debridement
88305
Skin, other than cyst/tag/debridement/plastic repair
Skin specimens have a limited number of codes. A gross-only skin specimen would be coded 88300, while skin from a plastic repair is 88302. A skin cyst, skin tag, or skin debridement is coded 88304 regardless of the size. All other skin specimens, including complex tissues such as excisions of melanoma and basal cell carcinoma with assessment of margins, fall under 88305, skin other than cyst, tag, debridement, or plastic repair. As such, a 4-mm punch biopsy of skin is an 88305 as would be an 8 × 4-cm skin excision for basal cell carcinoma with evaluation of the margins. When a portion of skin accompanies another specimen, such as the portion of skin surrounding a mastectomy or a bit of skin encompassing the biopsy tract from a soft tissue sarcoma resection, the skin portion is not usually coded in addition to the primary specimen unless there is some reason to do so. Such reasons may include additional pathology evident to the examining pathologist or specific instructions from the surgeon.
Breast
The codes for breast specimens are
88305
Breast, biopsy, not requiring microscopic evaluation of surgical margins
88305
Breast, reduction mammoplasty
88307
Breast, excision of lesion, requiring microscopic evaluation of surgical margins
88307
Breast, mastectomy—partial/simple
88309
Breast, mastectomy—with regional lymph nodes
We have already alluded to special cases with breast specimens. A reduction mammoplasty would be coded 88305. Of course, if you have separately identifiable bilateral reduction mammoplasties, you would have 88305 × 2. For a typical breast biopsy not requiring examination of the margins such as a needle biopsy or small incisional biopsy or an excisional discrete lesion such as fibroadenoma where the margin is not important, you would code 88305. For a biopsy where the margin is important, such as an excisional biopsy of an infiltrating carcinoma, 88307 is used since you need to evaluate and report the margins. A partial or simple mastectomy is also coded 88307, while a mastectomy with regional lymph nodes is 88309 even if you receive the axillary lymph nodes in a separate container from the breast tissue.
GYN Specimens
Gynecologic (GYN) specimens are coded using the following codes
88305
Endometrium, curettings/biopsy
88305
Polyp, cervical/endometrial
88305
Ovary, with/without tube, nonneoplastic
88305
Ovary, biopsy/wedge resection
88305
Uterus, with/without tubes and ovaries, for prolapse
88307
Cervix, conization
88307
Ovary, with/without tube, neoplastic
88307
Uterus, with/without tubes and ovaries, other than neoplastic/prolapse
88309
Uterus, with/without tubes and ovaries, neoplastic
For GYN specimens, 88305 is used to code endometrial curettings, biopsies, and polyps. A nonneoplastic ovary with or without its corresponding fallopian tube is also an 88305. For specimens representing a biopsy or wedge resection of an ovary, the code is 88305. A uterus for prolapse is an 88305, and because the description is with or without tubes and ovaries, use only a single 88305 code for a prolapsed uterus with tubes and ovaries. Even though this seems like a lot of tissue compared with an endometrial biopsy, codes are assigned based on average total work and closest match—in short, just follow the rules and code exactly as laid out in the CPT manual.
A cervical conization specimen is coded 88307 as is a neoplastic ovary with or without its corresponding fallopian tube. More work equals a higher code, generally speaking, but this is only true in an aggregate sense and does not apply to work expended on an individual case. Up-coding a particularly challenging nonneoplastic ovary is not allowed. There will be outliers on both ends of the coding spectrum. This is especially true for the 88305 code. If you have a nonneoplastic uterus with or without its adnexa that was not removed for prolapse (such as a specimen for endometriosis), it would be coded 88307. For a neoplastic uterus with or without tubes and ovaries, use the 88309. There is an exception to bundling together using the tubes and ovaries phrase for cases when the surgeon sends an ovary separately because of its own presumed pathology or if the gross findings indicate the ovary requires “separate and individual attention.” For example, if the surgeon is doing a total abdominal hysterectomy with bilateral salpingo-oopherectomy (TAH-BSO) for endometrial adenocarcinoma (88309) but sees a 3-cm mass in the left ovary and sends it to you for a frozen section which reveals a hemorrhagic corpus luteum (a nonneoplastic ovary, 88305), one would code 88309 for the neoplastic uterus plus 88305 for the nonneoplastic ovary plus a code for frozen section (FS, 88331) as we will learn later (Fig. 3.1).
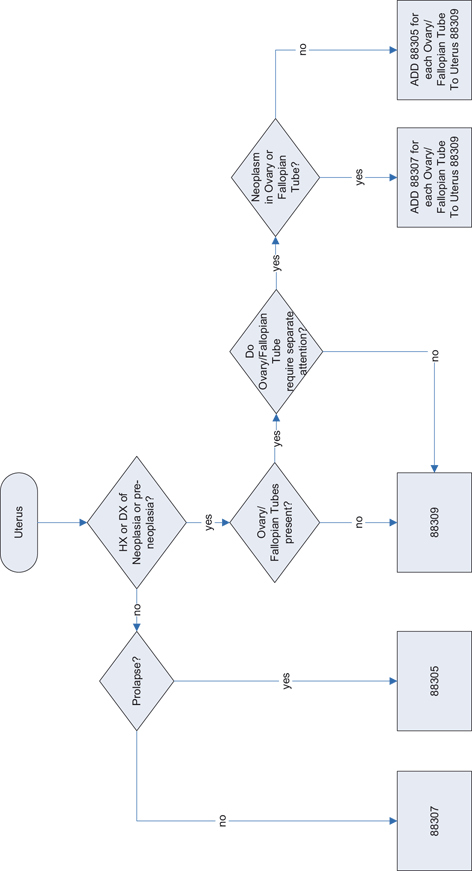

Fig. 3.1
Decision tree for Current Procedural Terminology (CPT) coding of uteri
Decalcification and Special Stains
For decalcification and special stains, the codes are
88311
Decalcification procedure (list separately in addition to code(s) for surgical pathology examination)
88312
Special stains including interpretation and report; Group I for microorganisms (e.g., acid fast, methenamine silver), each
88313
…Group II, all other (e.g., iron, trichrome), except stain for microorganisms, stains for enzyme constituents, or immunocytochemistry and immunohistochemistry
If you decalcify a specimen, you can code 88311 in addition to the specimen’s other code or codes. It does not matter how many blocks or pieces you decalcify of a specimen; it is just one code. Also make sure you document in your report that you decalcified something. Ultimately, every code you report must be backed up by the surgical pathology report; otherwise, your charges are subject to prospective or retrospective denial by government payers and private insurers alike.
Special stains for microorganisms are coded 88312, while non-microorganism histochemical stains are coded 88313. You are permitted to bill one unit of special stain charge per different stain per different tissue block or preparation. For example, a periodic acid-Schiff (PAS) for fungi and acid fast bacilli (AFB) on two different blocks of a lung resection are reported as four units of 88312, with proper documentation in the pathology report. Medical justification for special stains should appear in your report: Why did you order the stain (i.e., what were you looking for), and what did you learn from it? With a few exceptions here and there (e.g., muscle and renal biopsies), special stains should be ordered only after the routine sections (e.g., hematoxylin and eosin; H&E slides) are examined.
Immunohistochemical Staining
Immunohistochemical staining utilizes the following CPT codes:
88342
IHC or immunocytochemistry, per specimen; initial single antibody stain procedure
88341
Each additional single antibody stain procedure (list separately in addition to code for primary procedure)
88344
Each multiplex antibody stain procedure
(Author’s note: The fact that code 88341 follows 88342 in the preceding list is not a typographical error. The codes are out of numerical sequence in the official AMA codebook.)
Codes 88341 and 88342 apply when a pathologist reports an IHC stain using qualitative expression. A result is stated in qualitative terms if the report says simply that such and such a stain is positive or negative; for example, “the tissue stains negatively for cytokeratin” is a qualitative result .
Report one unit of 88342 for the initial qualitative single IHC antibody stain per different specimen. Report one unit of 88341 for each additional unduplicated single IHC stain (qualitative) documented for the same specimen. Note that, unlike special stain codes 88312 and 88313 discussed earlier in this chapter, the unit of service for IHC stains is the specimen, not the block or preparation. Furthermore, realize that if you are running a battery of several qualitative IHC stains on one specimen, it is totally arbitrary which one you think of as the “initial” stain for code 88342 reporting purposes.
Code 88344 comes into play when two or more separately interpretable antibodies can be simultaneously interrogated on one slide. You will encounter this situation mainly with an IHC multiplex stain such as prostatic intraepithelial neoplasia-4 (PIN-4, prostate) or the breast triple stain, which are single primary stains that come in one vial and require just one application, but they react to three unique antibodies by means of color and/or site (cell nucleus vs. cytoplasm) distinction. Typically, only one multiplex stain is performed per any given specimen .
Not every IHC multi-antibody, dual stain, or triple stain warrants reporting with code 88344. For code 88344 to be reported, the pathologist must be able to tell precisely which of two or three different antibodies is staining positive and which is not. Some IHC multi-antibody stains do not fulfill this requirement, such as AE1/AE3, which stains for two different antibodies, but the pathologist cannot tell whether it is the AE1, the AE3, or both that is/are positive in a given instance. The AMA instructs that an IHC “cocktail” stain be reported as a single-antibody stain (i.e., code 88342 or 88341) .
Qualitative IHC is separate and distinct from quantitative/semiquantitative IHC: The former is not part of the latter from either a clinical or a billing perspective. Accordingly, it is never appropriate to report code 88341 or 88342 together with code 88360 or 88361 (see next paragraph) for the same IHC staining procedure on the same specimen. Furthermore, it would not be medically necessary to perform the same IHC stain by both qualitative and quantitative approach on the same specimen.
Two CPT codes are used for reporting quantitative and semiquantitative IHC or immunocytochemistry used to detect antigens in tissue.
88360
Morphometric analysis, tumor IHC (e.g., Her-2/neu, estrogen receptor (ER), progesterone receptor (PR)), quantitative or semiquantitative, per specimen, each single antibody stain procedure; manual
88361
Using computer-assisted technology
Codes 88360 and 88361 apply when a quantitative or semiquantitative result is determined and reported using the IHC staining technique. Quantitative/semiquantitative results are derived by counting the number of positive cells and expressing the outcome as a number, such as a “score” or the percentage of positive cells. A common method of “scoring” Her-2/neu IHC involves counting positive cells to a threshold number like 30 %, combined with a subjective assessment of staining intensity:The 0–3 + score is deemed to be a semiquantitative result (CAP Today, February 2005). Report code 88361 for the IHC test if the counting is computer assisted, but for manual-counting method, report code 88360 .
Pathologists frequently base their interpretation of a semiquantitative IHC stain on a visual approximation of the percentage of positive cells instead of actually counting cells. Practice guidance published by the College of American Pathologists confirms that, as regards the evaluation of IHC stains, the term “semiquantitative” covers a determination made by visual approximation as well as one made by literally counting positive cells (Protocol for the Examination of Specimens from Patients with Invasive Carcinoma of the Breast, CAP, October 2009).
The approved unit of service for codes 88360 and 88361 is each different single or multiplex antibody stain procedure per each different specimen. For example, a Her-2/neu, ER, PR, and Ki-67 by manual tumor morphometry on bilateral breast biopsies would be reported as 88360 × 8 (four different stains on each of two different specimens); however, the same four stains on two different blocks of the same specimen would yield just four units of 88360 .
Intraoperative Consultation Codes
88329
Pathology consultation during surgery
88331
First tissue block, with frozen section(s), single specimen
88332
Each additional tissue block with frozen section(s)
88333
Cytologic preparation exam, first site, single specimen
88334
Cytologic preparation exam, each additional site, single specimen
For a gross-only type consultation , such as grossly evaluating a margin, the code is 88329. For frozen sections, the first tissue block frozen for any specimen is an 88331; any additional blocks from that specimen are coded 88332. For example, for a skin excision for which you freeze and interpret four blocks to determine the margins, you would code 88331 × 1 and 88332 × 3. If the four margins have been submitted separately and separately designated by the surgeon, they would represent four different specimens which would yield total codes of 88331 × 4. Once again, clear documentation of what was done is critical to ensure payment.
Intraoperative consultation by microscopic examination of a cytologic preparation (e.g., touch preparation or squash preparation) is reported with codes 88333 (first site per specimen) and 88334 (each additional site per specimen). If you examine four margins of a lumpectomy specimen using touch preparation (one slide per margin), you would report that as 88333 for the first margin and 88334 for each additional margin (e.g., 88334 × 3 for this example) . It is completely arbitrary which margin you think of as the “first” margin from a CPT code perspective.
Some specimens, such as a lymph node, do not have margins per se, so two touch preparations examined intraoperatively for such a specimen warrant only one charge (i.e., 88333 alone). However, if two lymph nodes are presented to you as a single specimen for intraoperative examination, that would support an 88333 plus an 88334 coding scenario. Again, your report documentation is critical to correct CPT coding and third-party payer audit support.
You can report frozen section code 88331 and touch preparation code 88334 together for the same specimen in some instances. For example, you might examine the primary lesion in a lumpectomy specimen via frozen section and then separately examine three margins using touch preparation technique. With proper report documentation, you would report that as 88331 for the frozen section intraoperative diagnosis and 88334 × 3 for the cytologic preparation examination of three surgical margins. Never report codes 88331 and 88333 together for the same specimen .
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


