Attention Deficit/Hyperactivity Disorder
KEY CONCEPTS
![]() Untreated or ineffectively treated childhood attention deficit/hyperactivity disorder (ADHD) can lead to poor school performance, poor socialization, and increased risk for traffic accidents, psychiatric comorbidities, unemployment, and incarceration during adolescence and adulthood.
Untreated or ineffectively treated childhood attention deficit/hyperactivity disorder (ADHD) can lead to poor school performance, poor socialization, and increased risk for traffic accidents, psychiatric comorbidities, unemployment, and incarceration during adolescence and adulthood.
![]() ADHD is 80% genetic in origin, and it is associated with decreased brain volume, a delay in cortical thickening, and dysregulation of the “default mode network,” a brain system that regulates attention, prioritization of information, memory, and impulse control.
ADHD is 80% genetic in origin, and it is associated with decreased brain volume, a delay in cortical thickening, and dysregulation of the “default mode network,” a brain system that regulates attention, prioritization of information, memory, and impulse control.
![]() Symptoms of inattention or hyperactivity and impulsivity or all three must be present during childhood and cause functional impairment in two different settings for 6 months to meet diagnostic criteria for ADHD.
Symptoms of inattention or hyperactivity and impulsivity or all three must be present during childhood and cause functional impairment in two different settings for 6 months to meet diagnostic criteria for ADHD.
![]() Pretreatment assessment of overall physical and mental health, psychiatric comorbidities, and goals of treatment must be set prior to initiating pharmacotherapy.
Pretreatment assessment of overall physical and mental health, psychiatric comorbidities, and goals of treatment must be set prior to initiating pharmacotherapy.
![]() Preschoolers, school-age children, adolescents, and adults with ADHD all can benefit from nonpharmacologic interventions that include a healthy diet, education on ADHD, and potentially effective cognitive and behavioral treatments.
Preschoolers, school-age children, adolescents, and adults with ADHD all can benefit from nonpharmacologic interventions that include a healthy diet, education on ADHD, and potentially effective cognitive and behavioral treatments.
![]() The psychostimulants, methylphenidate or amphetamine salts, are the most effective pharmacologic treatment options for all ages with a rapid therapeutic effect, typically within 1 or 2 hours of an effective dose.
The psychostimulants, methylphenidate or amphetamine salts, are the most effective pharmacologic treatment options for all ages with a rapid therapeutic effect, typically within 1 or 2 hours of an effective dose.
![]() α2-Adrenergic agonists such as extended-release preparations of guanfacine and clonidine are less effective than stimulants in monotherapy and are used as adjuncts to improve symptom control, particularly oppositional behaviors and insomnia.
α2-Adrenergic agonists such as extended-release preparations of guanfacine and clonidine are less effective than stimulants in monotherapy and are used as adjuncts to improve symptom control, particularly oppositional behaviors and insomnia.
![]() When ADHD coexists with bipolar disorder, it is necessary to first stabilize the mood with lithium, an anticonvulsant, or an atypical antipsychotic before adding an ADHD-specific medication such as a psychostimulant.
When ADHD coexists with bipolar disorder, it is necessary to first stabilize the mood with lithium, an anticonvulsant, or an atypical antipsychotic before adding an ADHD-specific medication such as a psychostimulant.
![]() When ADHD coexists with other psychiatric conditions, such as anxiety disorders, major depression, or Tourette’s disorder, it is optimal to treat the most functionally impairing disorder first (whether it is ADHD or the co-occurring condition) and then treat the second disorder.
When ADHD coexists with other psychiatric conditions, such as anxiety disorders, major depression, or Tourette’s disorder, it is optimal to treat the most functionally impairing disorder first (whether it is ADHD or the co-occurring condition) and then treat the second disorder.
![]() Atomoxetine is a good option to manage ADHD symptoms in adolescents and adults with substance abuse disorders. It has a delayed onset of effect (2 to 4 weeks), but it has no abuse potential.
Atomoxetine is a good option to manage ADHD symptoms in adolescents and adults with substance abuse disorders. It has a delayed onset of effect (2 to 4 weeks), but it has no abuse potential.
INTRODUCTION
Once considered primarily a childhood disorder, attention deficit/hyperactivity disorder (ADHD) is now known to persist into adolescence for 75% and into adulthood for approximately 50% of individuals.1,2 The American Academy of Pediatrics (AAP) considers ADHD a chronic condition that requires ongoing management.1 Functionally impairing inattention, impulsivity, and hyperactivity in the ADHD brain have been correlated with neuroanatomical and functional brain changes.3,4 It is unusual for an individual to display signs of the disorder in all settings or even in the same setting at all times; however, there is a persistent pattern of symptoms that persists for 6 months or more.3,5 Co-occurring anxiety, mood disorders, learning disabilities, medical conditions, and substance abuse must be considered in assessment and treatment. Behavioral interventions and medications are effective for all ages, but there are special considerations for treatment plan development and monitoring in each age group.1–3
The psychiatric assessment of a child requires obtaining information from the child, parents, caregivers, and teachers.1 Treating children with psychotropic drugs requires a very different approach than treating adults. Children undergo neurologic, physiologic, and psychosocial changes throughout development. Age-related pharmacodynamic and pharmacokinetic differences can alter drug disposition and response. Psychotropic drug treatment of children is intended to control symptoms or behaviors that impair learning and development.1,3 Children may not be able to articulate symptom response or adverse effects of a medication. ![]() Adolescents and adults with ADHD may not have been diagnosed and treated during childhood, putting them at greater risk for the psychosocial consequences of ADHD including unemployment, unstable relationships, substance abuse, and incarceration.1–3,6,7
Adolescents and adults with ADHD may not have been diagnosed and treated during childhood, putting them at greater risk for the psychosocial consequences of ADHD including unemployment, unstable relationships, substance abuse, and incarceration.1–3,6,7
EPIDEMIOLOGY
In 2010, 5 million children in the United States aged 3 to 17 years had ADHD (8%). Boys (11%) were about twice as likely as girls (6%) to have ADHD. Non-Hispanic white and black children were more likely to have ADHD compared with children of Hispanic or Asian descent.8 Worldwide rates of ADHD in children range from 4% to 12%.3 Several epidemiologic studies, including surveys conducted by the National Institutes of Health (NIH), have documented rates of adult ADHD between 3% and 5% with comparable rates in men and women.2,3
Prescriptions for ADHD medication increased in all age groups from 1998 to 2005, particularly in adolescents and young adults.3,9 A National Poison Control Center study estimated that between 1998 and 2005, prescriptions for teenagers and preteenagers increased 133% for amphetamine products, 52% for methylphenidate products, and 80% for both.9 The FDA used prescription records from 59,000 retail pharmacies to analyze prescribing rates in 2010 compared with those in 2002 in children aged 0 to 17 years for several therapeutic areas including antibiotics, proton-pump inhibitors, antidepressants, and ADHD medications. Overall pediatric prescribing decreased 7% over the 8 years studied, but prescriptions for ADHD medications increased by 46%. Methylphenidate was the most commonly prescribed drug in the ADHD category, but usage remained constant from 2002 to 2010, whereas usage of amphetamine products dropped by 15%.10 Usage of dexmethylphenidate, lisdexamfet-amine, and guanfacine increased from 2004 to 2010, while usage of atomoxetine in youth decreased.10
ETIOLOGY AND PATHOPHYSIOLOGY
![]() Both genetic and nongenetic factors are implicated in the pathogenesis. First-degree relatives of an individual with ADHD have a fourfold to eightfold increased chance of developing ADHD compared with the general population; mean heritability (the proportion of variance due to genetics) is around 80%.11 Candidate gene studies have implicated the dopamine transporter and receptor genes as well as the SNAP25 and COMT genes, but they have been found to account for only a small portion of the variance in ADHD symptoms. Genome-wide association studies (GWAS) have suggested that 40 to 80 different genes might be involved in ADHD, each conveying a small degree of risk.12
Both genetic and nongenetic factors are implicated in the pathogenesis. First-degree relatives of an individual with ADHD have a fourfold to eightfold increased chance of developing ADHD compared with the general population; mean heritability (the proportion of variance due to genetics) is around 80%.11 Candidate gene studies have implicated the dopamine transporter and receptor genes as well as the SNAP25 and COMT genes, but they have been found to account for only a small portion of the variance in ADHD symptoms. Genome-wide association studies (GWAS) have suggested that 40 to 80 different genes might be involved in ADHD, each conveying a small degree of risk.12
GWAS studies have previously focused on common variants, assuming a small number of genetic alterations, common in the population, accounted for most of the genetic risk in ADHD; this is clearly not the case.13 Recently genetic studies have focused on multiple rare variants, that is, hundreds or even thousands of genetic variants might be involved in ADHD, such that each patient has a unique genetic pattern. Patients might have copies or deletions in the genome that cover multiple genes called copy number variants (CNV). These CNV studies have implicated a number of systems in ADHD: cholinergic receptors, cholesterol metabolism, and genes for CNS development,14 an area of chromosome 15q13,15 as well as glutamate metabotropic receptors.16 Thus, the pathophysiology of ADHD may go well beyond the catecholamine systems that have been the focus of most studies to date.
Environmental factors may be involved in the etiology of ADHD, as well. Children with fetal alcohol syndrome, lead poisoning, and meningitis have a higher incidence of ADHD symptomatology.3,17 ADHD is associated with a variety of environmental risks, including obstetric adversity, maternal smoking, and adverse parent–child relationships.3,17
![]() Although there are no definitive pathophysiologic markers for ADHD, imaging studies show subjects with ADHD have decreased total brain volume relative to controls in multiple brain regions (right prefrontal cortex, caudate nucleus, anterior cingulate gyrus, and cerebellum). Global thinning of the cortex has been observed in children with ADHD, and comparative studies show there is a delay in cortical thickening in ADHD brains relative to age-matched controls.3 There is evidence showing that adults with ADHD whose symptoms remitted over time have increased cortical thickening and greater brain volume in key regions controlling attention and behavior than those with residual ADHD symptoms across adulthood.18
Although there are no definitive pathophysiologic markers for ADHD, imaging studies show subjects with ADHD have decreased total brain volume relative to controls in multiple brain regions (right prefrontal cortex, caudate nucleus, anterior cingulate gyrus, and cerebellum). Global thinning of the cortex has been observed in children with ADHD, and comparative studies show there is a delay in cortical thickening in ADHD brains relative to age-matched controls.3 There is evidence showing that adults with ADHD whose symptoms remitted over time have increased cortical thickening and greater brain volume in key regions controlling attention and behavior than those with residual ADHD symptoms across adulthood.18
Functional magnetic resonance imaging (MRI) studies during inhibitory control tasks in patients with ADHD show reduced activity in prefrontal and anterior cingulate cortex, deficits which may be reversed with stimulant treatment.19,20 Adults and children with ADHD show decreased activation of the ventral striatum when anticipating reward.21,22 ![]() Alterations in the “default mode” attention network have been found in adults with ADHD.3 The default mode network consists of the medial prefrontal cortex, medial parietal lobe or precuneus, as well as the posterior cingulate. These areas are active during the “resting state” when attention is not engaged; this system is actively suppressed during active attention. A lack of connectivity between the prefrontal cortex and precuneus (located in the midline of the parietal lobe) is associated with failure of suppression of the default mode network, causing lapses in attention and inhibitory control.23 Recently, methylphenidate has been shown to decrease aberrant default mode network activation in children with ADHD.24
Alterations in the “default mode” attention network have been found in adults with ADHD.3 The default mode network consists of the medial prefrontal cortex, medial parietal lobe or precuneus, as well as the posterior cingulate. These areas are active during the “resting state” when attention is not engaged; this system is actively suppressed during active attention. A lack of connectivity between the prefrontal cortex and precuneus (located in the midline of the parietal lobe) is associated with failure of suppression of the default mode network, causing lapses in attention and inhibitory control.23 Recently, methylphenidate has been shown to decrease aberrant default mode network activation in children with ADHD.24
CLINICAL PRESENTATION
The AAP guideline for the diagnosis, evaluation, and treatment of ADHD in children and adolescents recommends an evaluation for any child 4 to 18 years of age who presents with academic or behavioral problems and symptoms of inattention, hyperactivity, or impulsivity.1 ![]() At least six symptoms of inattention or hyperactivity and impulsivity causing impairment in more than one major setting for 6 months and an onset of symptoms before age 7 are currently required by the Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition, Text Revision (DSM-IV-TR) for a diagnosis of ADHD.5 Validated rating scales, such as the Connors Rating Scales—revised (CRS-revised), are recommended for objective symptom ratings from parents and teachers in different age groups.1,3,7 The age criteria will likely be raised to 12 years old in the fifth edition of the DSM (DSM-5), given that cases of ADHD without prominent hyperactivity may be missed in childhood.25 The DSM-5 may lower the number of symptoms required to make a diagnosis in adolescents and adults, given that epidemiologic studies have shown that adolescents and adults have fewer numbers of symptoms than children, but the symptoms are just as impairing.2,7,26 These proposed changes in the DSM-5 are controversial, as some are concerned that they may result in a dramatic increase in diagnosis of ADHD and an increase in the prescribing of ADHD medications.27 To make a diagnosis of ADHD, the clinician should rule out alternative causes of symptoms (learning disability, situational stressor) and assess for other conditions that may coexist with ADHD including oppositional defiant and conduct disorders, tics, and sleep and mood disorders.
At least six symptoms of inattention or hyperactivity and impulsivity causing impairment in more than one major setting for 6 months and an onset of symptoms before age 7 are currently required by the Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition, Text Revision (DSM-IV-TR) for a diagnosis of ADHD.5 Validated rating scales, such as the Connors Rating Scales—revised (CRS-revised), are recommended for objective symptom ratings from parents and teachers in different age groups.1,3,7 The age criteria will likely be raised to 12 years old in the fifth edition of the DSM (DSM-5), given that cases of ADHD without prominent hyperactivity may be missed in childhood.25 The DSM-5 may lower the number of symptoms required to make a diagnosis in adolescents and adults, given that epidemiologic studies have shown that adolescents and adults have fewer numbers of symptoms than children, but the symptoms are just as impairing.2,7,26 These proposed changes in the DSM-5 are controversial, as some are concerned that they may result in a dramatic increase in diagnosis of ADHD and an increase in the prescribing of ADHD medications.27 To make a diagnosis of ADHD, the clinician should rule out alternative causes of symptoms (learning disability, situational stressor) and assess for other conditions that may coexist with ADHD including oppositional defiant and conduct disorders, tics, and sleep and mood disorders.
Clinical Controversy…
CLINICAL PRESENTATION ADHD
Preschoolers (3 to 5 Years)
The DSM-IV-TR diagnostic criteria for ADHD can be applied to preschool-age children, although it may be difficult to document symptoms in multiple settings with different caregivers if the child does not attend preschool.28,29 Enrollment in a qualified preschool and a parent training program is often recommended. Both can help parents develop reasonable expectations for their child’s development and foster the development of management skills for problem behaviors. Although methylphenidate has been found safe and effective for ADHD in 4- and 5-year-olds, behavioral interventions are recommended first. Medications can be considered when the child has moderate to severe symptoms unresponsive to behavioral interventions. The clinician needs to weigh the risks of starting medication at an early age against the harm of delaying diagnosis and treatment.1
School Age (6 to 11 Years)
Most cases of ADHD are first realized during ages 6 to 9 years, with the child having difficulty academically and/or socially in school and at home. Most children have combined inattentive and hyperactive or impulsive symptoms that cause functional impairment. This period is crucial to the child’s success in school, socialization, and the development of his or her sense of self; therefore, accurate diagnosis and treatment is critical. Comorbid oppositional defiant disorder (ODD), conduct disorder, and aggression are indicators that the child is at greater risk for delinquency and substance abuse in adolescence.30,31 This is the most well-studied age group, with strong data showing benefits of recognition and treatment with behavioral interventions and medications.1
Adolescents (12 to 18 Years)
Hyperactivity decreases in adolescents, and inattention and impulsivity are the more prominent functionally impairing symptoms. There may be fewer numbers of symptoms of ADHD in adolescence, but the symptoms present cause significant functional impairment.26 Higher rates of delinquency, drug and alcohol use, and psychiatric comorbidity have been documented in adolescents with ADHD compared with in those without ADHD.1,6,7,26 Assessment for substance abuse and risk of diversion must be considered before starting stimulant medications. Speeding and increased motor vehicle accidents occur at higher rates in teens with ADHD compared within those without the disorder.1,6
Adults
The presence of multiple comorbid conditions, particularly conduct or mood disorder, can increase the likelihood of ADHD chronicity into adulthood. DSM-IV-TR criteria for ADHD in childhood also apply to adults. Inattentive symptoms are the most common and functionally impairing in adults, but hyperactive and impulsive symptoms are experienced by many and are associated with higher rates of bipolar disorder and psychosis.2 Cognitive deficits (e.g., executive functioning, working memory, task prioritization, lower IQ) have been documented in adults with ADHD in addition to a greater risk for unstable relationships, unemployment, psychiatric hospitalization, and incarceration compared with those without ADHD.2,7,32 An ADHD screening tool is available to facilitate assessment in adults not diagnosed during childhood (http://www.addcoach4u.com/documents/adultadhdscreenertest1.pdf).33
TREATMENT
ADHD-specific cognitive and behavioral interventions are increasingly recognized as necessary components of an overall treatment plan aimed at symptom relief and optimal functioning. Several studies show combining medications with behavioral interventions produces the greatest symptom relief and the best outcomes.
Desired Outcomes
![]() Specific goals of treatment or desired outcomes must be identified (e.g., able to sit in chair for 20 minutes; completes homework assignments, or no longer blurts out comments in class without being called upon). For adults, the desired outcome may be to read an entire newspaper before starting another project, improving safety while driving, or successfully completing tasks on time at work.2,17,32
Specific goals of treatment or desired outcomes must be identified (e.g., able to sit in chair for 20 minutes; completes homework assignments, or no longer blurts out comments in class without being called upon). For adults, the desired outcome may be to read an entire newspaper before starting another project, improving safety while driving, or successfully completing tasks on time at work.2,17,32
Nonpharmacologic Therapy
Educational, Cognitive, and Behavioral Interventions
![]() Education on ADHD as a biologic disorder with brain-derived causes is essential for destigmatizing ADHD and improving treatment acceptance. Parent training and behavioral interventions such as positive rewards for good behavior and structured limit setting are recommended as first-line interventions before medication trials in preschoolers (3- to 5-year-olds) with ADHD. Behavioral interventions for ADHD are described in Table 46-1. It is crucial to get parents, teachers, and clinicians involved to coordinate care and provide consistent behavioral management for the child at home and at school. School-age children (6 to 11) also benefit from these behavioral interventions in addition to strategies, such as breaking up homework assignments into shorter, manageable segments. Although it varies by state, children and adolescents with ADHD may qualify for an individualized educational program (IEP) that allows for more time to take an exam, preferred seating, and modified work assignments.1,28 It is noteworthy that most studies comparing behavioral intervention with stimulant therapy in youth found a much stronger effect on ADHD core symptoms from stimulants.1,3,4 Combined behavioral and stimulant therapy resulted in greater improvements on academic and conduct measures in some studies with greater parent and teacher satisfaction ratings. Combining behavioral interventions with stimulants may allow for lower doses of stimulant that can reduce the risk of adverse effects.1
Education on ADHD as a biologic disorder with brain-derived causes is essential for destigmatizing ADHD and improving treatment acceptance. Parent training and behavioral interventions such as positive rewards for good behavior and structured limit setting are recommended as first-line interventions before medication trials in preschoolers (3- to 5-year-olds) with ADHD. Behavioral interventions for ADHD are described in Table 46-1. It is crucial to get parents, teachers, and clinicians involved to coordinate care and provide consistent behavioral management for the child at home and at school. School-age children (6 to 11) also benefit from these behavioral interventions in addition to strategies, such as breaking up homework assignments into shorter, manageable segments. Although it varies by state, children and adolescents with ADHD may qualify for an individualized educational program (IEP) that allows for more time to take an exam, preferred seating, and modified work assignments.1,28 It is noteworthy that most studies comparing behavioral intervention with stimulant therapy in youth found a much stronger effect on ADHD core symptoms from stimulants.1,3,4 Combined behavioral and stimulant therapy resulted in greater improvements on academic and conduct measures in some studies with greater parent and teacher satisfaction ratings. Combining behavioral interventions with stimulants may allow for lower doses of stimulant that can reduce the risk of adverse effects.1
TABLE 46-1 Behavioral Interventions for ADHD

![]() Recommended behavioral interventions for adolescents and adults include keeping an external organizer (e.g., smart phone, notebook with “to-do” lists) and breaking up activities into short, manageable tasks. Recognizing triggers for distraction and making a point of thinking before acting are useful interventions and are recommended during cognitive behavioral therapy (CBT) sessions designed to manage adult ADHD.34,35 Establishing a regular schedule that includes exercise and relaxation can be beneficial as well. Controlled studies have shown that ADHD-specific CBT was more effective than psychoeducation and relaxation in adults with ADHD whose symptoms were only partially responsive to medication.34 Similarly, adults with ADHD that partially responded to medications benefited more from a group-administered metacognition program (2 h/wk over 12 weeks) compared with supportive therapy sessions administered for the same amount of time.35 The metacognitive therapy was designed to develop organizational skills and executive function self-management skills. Yoga, meditation, and some dietary supplements have been recommended for ADHD as well, but they should not take the place of more established effective treatments, such as medications and cognitive interventions.
Recommended behavioral interventions for adolescents and adults include keeping an external organizer (e.g., smart phone, notebook with “to-do” lists) and breaking up activities into short, manageable tasks. Recognizing triggers for distraction and making a point of thinking before acting are useful interventions and are recommended during cognitive behavioral therapy (CBT) sessions designed to manage adult ADHD.34,35 Establishing a regular schedule that includes exercise and relaxation can be beneficial as well. Controlled studies have shown that ADHD-specific CBT was more effective than psychoeducation and relaxation in adults with ADHD whose symptoms were only partially responsive to medication.34 Similarly, adults with ADHD that partially responded to medications benefited more from a group-administered metacognition program (2 h/wk over 12 weeks) compared with supportive therapy sessions administered for the same amount of time.35 The metacognitive therapy was designed to develop organizational skills and executive function self-management skills. Yoga, meditation, and some dietary supplements have been recommended for ADHD as well, but they should not take the place of more established effective treatments, such as medications and cognitive interventions.
Dietary Interventions
Extensive research has evaluated dietary interventions for ADHD, primarily in children with some adolescent data. When iron and zinc are supplemented in youth with known deficiencies, the therapeutic benefit of stimulant therapy can be enhanced, frequently allowing lower effective doses.36,37 Omega-3 supplements can benefit some individuals with few side effects, but results are not consistently better than placebo. Additive-free and oligoantigenic elimination diets (e.g., omitting red/orange food dye in lunch meat and hot dogs; avoiding allergenic foods such as dairy and wheat) have been found useful only in small numbers of children who do not respond to other interventions. Although scientific evidence is lacking, there is a universal belief among families that the avoidance of sugar and artificial sweeteners improves ADHD symptoms. The attention paid to sugar avoidance and healthy diet is the more likely reason for improved behavior. An overall healthy diet with the proper balance of protein, fresh produce, and fiber is recommended.37
Pharmacologic Therapy
Figure 46-1 provides an algorithm for drug selection in the treatment of ADHD.
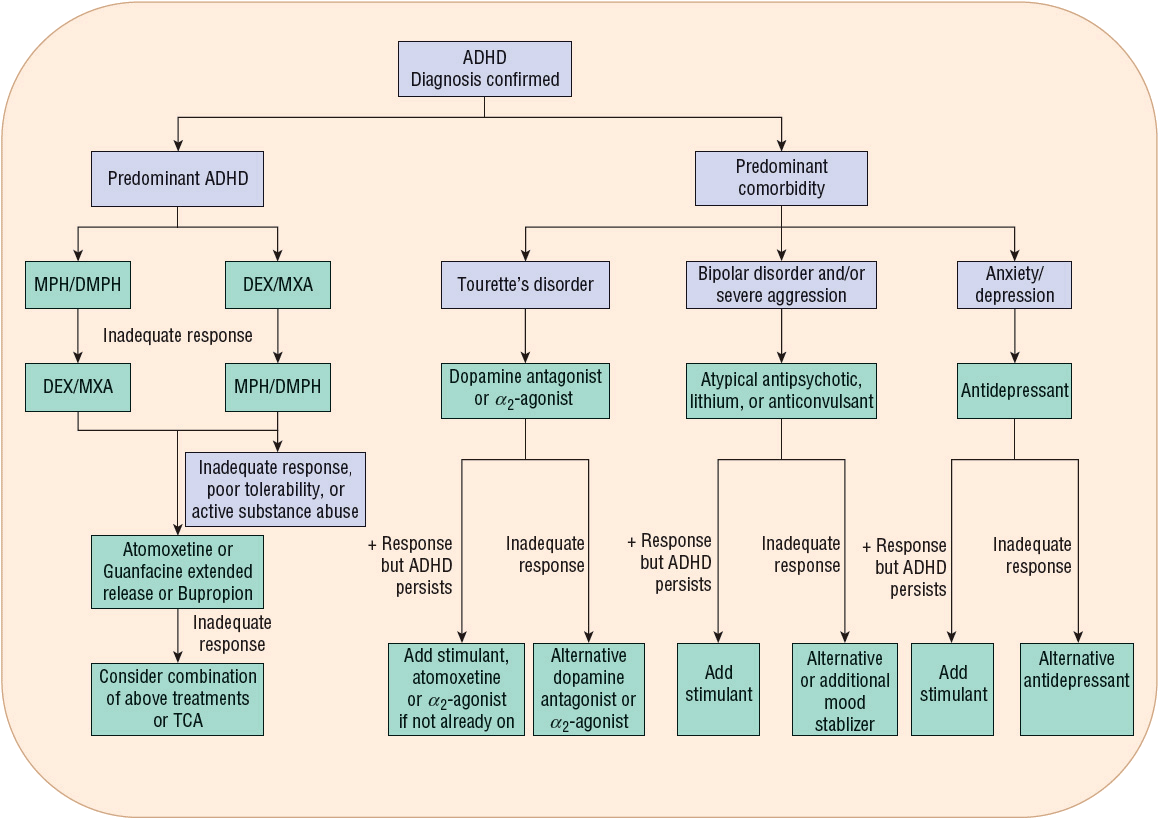
FIGURE 46-1 Algorithm for drug selection in the management of attention deficit/hyperactivity disorder (ADHD). Treat predominant disorder first, reassess, and consider alternative or adjunct medications for optimal symptom control. (DEX, dextroamphetamine; DMPH, dexmethylphenidate; MPH, methylphenidate; MXA, mixed amphetamine salts; TCA, tricyclic antidepressant.) (Data from references 3, 17, 45, 61, 63, 64, and 68.)



