The proximal aspect of the canal is defined by the anorectal ring, comprised of the proximal aspects of the internal and external sphincter muscles as well as the puborectalis muscle (Fig. 17.1b). This important ring forms the junction between the rectum and the anal canal and is critically important during the treatment of perianal sepsis as division of this ring would inevitably affect continence. The distal aspect of the anal canal is the anal verge, defined as the area where anoderm becomes true skin characterized by pigmentation, hair, sweat glands and a ring of apocrine glands, which may contribute to the condition hidradenitis suppurativa.
Anal Glands
Because of the diminishing size calibre from rectum to anus, the undulated dentate line area of the anal canal is characterized by a pleated appearance, which is referred to as the columns of Morgagni. At the base of each column, at the level of the dentate line, there is a small pocket or crypt. About half of these crypts communicate with the drainage ducts of anal glands that are located in the internal sphincter muscle area. These anal glands, which were first described by Hermann and Desfosses in 1844 [3], are located in the submucosal space, the internal sphincter muscle itself, and about half also communicate with the intersphincteric space, without involving the external sphincter muscle. Anal crypts are therefore of significant importance in the pathophysiology of anal sepsis as foreign material lodging itself in a crypt can obstruct the drainage path of anal glands and result in sepsis. The importance of this mechanism was first described by Parks in 1961 [4].
Perianal Spaces
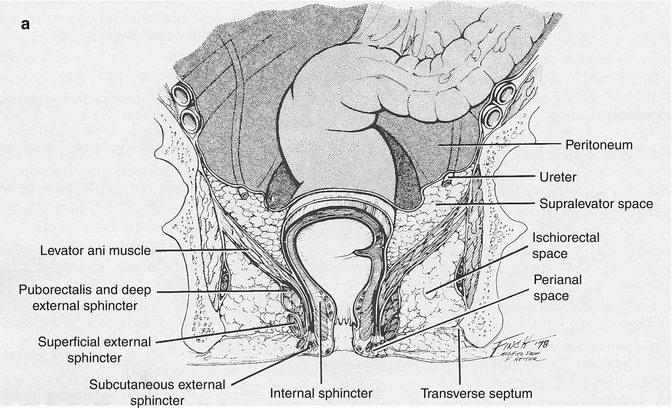
The complex of muscles which surround and form the anal canal create a network of spaces that are of paramount importance in the management of perianal sepsis (Fig. 17.2a).
The perianal space is in the immediate area of the anal verge surrounding the anal canal. The lateral aspect is continuous with the subcutaneous fat of the buttocks, while medially, it extends into the anal canal to the dentate line. It includes the distal most aspect of the external sphincter muscle and communicates freely with the intersphincteric space. The space is itself divided by an array of radiating elastic septa that limit communication within the space and account for the severe pain produced by the accumulation of even a small amount of pus.
The intersphincteric space is the space between the internal and external sphincter muscles. Proximally it terminates in the rectal wall, while distally, it communicates with the perianal space. This is the space that is often first seeded by sepsis of cryptoglandular origin.
The ischiorectal space or fossa is delineated proximally by the levator ani muscle and extends distally to the skin of the perineum. Laterally, along the obturator foramen, it contains Alcock’s canal which carries the internal pudendal vessels and nerve.
The supralevator spaces are located proximal to the levator muscle on either side of the rectum. They extend proximally or superiorly to the peritoneal reflection and are limited laterally by the pelvic wall. Sepsis in this area may come from upward extension of perianal sepsis or downward extension of pelvic sepsis. Differentiating the source of sepsis in this space is important for deciding the appropriate route of drainage.
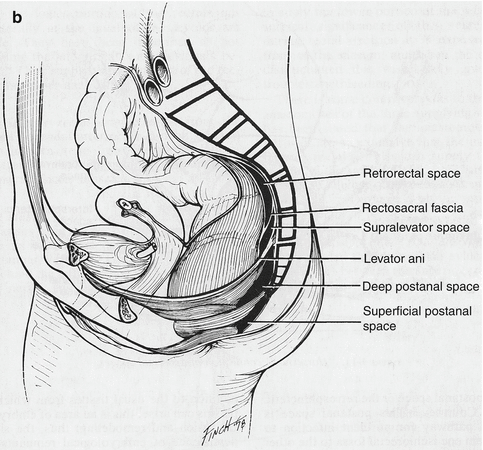
The postanal space is directly posterior to the anal canal and altogether distal to the levator ani muscle (Fig. 17.2b). It is divided into deep and superficial postanal space based on whether it is deep or superficial to the anococcygeal ligament. This space is of significant importance for understanding the pathophysiology of bilaterally communicating ischiorectal space sepsis, also known as a horseshoe abscess.
Pathophysiology
Anorectal sepsis is a common condition that can occur in healthy, normal individuals. Since anorectal abscesses often lead to fistulae formation, it is reasonable to consider both on the same pathological continuum.
Aetiology
There are several reasons that can account for the development of anal sepsis. Most commonly, the cause is of cryptoglandular origin, whereby anal crypts are obstructed and the drainage path of anal gland secretions is blocked. As a result, pus accumulates and builds in a retrograde fashion often seeding the intersphincteric space [5]. Other notable causes of perianal sepsis include perianal trauma and anal foreign bodies, which can cause abscess formation by the same mechanism as inspissated faecal material in anal crypts. Iatrogenic causes such as surgical wounds, haemorrhoid banding or injection have also been reported to occasionally cause perianal sepsis. More recently, two reviews have been published on stapled hemorrhoidectomy as another potential cause of severe perianal, pelvic and even intra-abdominal sepsis [6, 7]. Lastly, skin lesions such as hidradenitis suppurativa, localized pyoderma or infection of a sebaceous adenoma are also possible causes of perianal sepsis. Crohn’s disease, while not itself a cause, is a strongly predisposing factor in the development of perianal abscesses, usually via the cryptoglandular mechanism.
Anal fistulas are also predominantly of cryptoglandular origin and will develop in approximately one-third of patients who undergo drainage of an anorectal abscess. A recent retrospective cohort study of 148 patients with anorectal abscesses showed a 37 % overall rate of fistula formation over a mean follow-up period of 38 months and a twofold increased risk of fistula formation in patients under the age of 40 [8]. While about 90 % of fistulas have a cryptoglandular aetiology, not all fistulas come from antecedent abscesses, and not all abscesses lead to fistula formation. Indeed a previous history of abscess may not be elicited in one-third of patients with anal fistula [9]. The remaining 10 % of anal fistulas have the following specific aetiologies (Table 17.1): anorectal disease, inflammatory bowel disease, infection, malignancy and trauma. It is important to distinguish the aetiology of an anal fistula in order to provide adequate treatment. Indeed, perianal fistulizing disease may be the initial presentation in 10 % of Crohn’s patients, preceding the diagnosis by several years, and remains the only manifestation of disease in about 5 % of patients [10].
Table 17.1
Aetiology of anorectal fistulas
Nonspecific (90 %) | Cryptoglandular |
Specific (10 %) | Crohn’s disease |
Chronic ulcerative colitis | |
Trauma | |
Foreign body | |
Carcinoma (anal Ca, rectal Ca) | |
Leukaemia/lymphoma | |
Radiation | |
Tuberculosis | |
Lymphogranuloma granulosum | |
Actinomycosis
Stay updated, free articles. Join our Telegram channel
Full access? Get Clinical Tree
 Get Clinical Tree app for offline access
Get Clinical Tree app for offline access

|