Acne Vulgaris
KEY CONCEPTS
![]() Acne is a highly prevalent disorder affecting many adolescents and adults.
Acne is a highly prevalent disorder affecting many adolescents and adults.
![]() It is an extremely complex disease with an etiology originating from multiple causative and contributory factors.
It is an extremely complex disease with an etiology originating from multiple causative and contributory factors.
![]() Elements of pathogenesis involve defects in epidermal keratinization, androgen secretion, sebaceous function, bacterial growth, inflammation, and immunity.
Elements of pathogenesis involve defects in epidermal keratinization, androgen secretion, sebaceous function, bacterial growth, inflammation, and immunity.
![]() Acne vulgaris cannot be “cured.” Goals of treatment of this chronic disorder include control and alleviation of symptoms by reducing the number and severity of lesions, slowing progression, and limiting disease duration and recurrence. Key elements for patient adherence to therapy include prevention of long-term disfigurement associated with scarring and hyperpigmentation and avoidance of psychologic suffering.
Acne vulgaris cannot be “cured.” Goals of treatment of this chronic disorder include control and alleviation of symptoms by reducing the number and severity of lesions, slowing progression, and limiting disease duration and recurrence. Key elements for patient adherence to therapy include prevention of long-term disfigurement associated with scarring and hyperpigmentation and avoidance of psychologic suffering.
![]() The most critical target for treatment is the microcomedone, as the entire pathogenic cascade of acne is arrested if follicular occlusion is minimized or reversed. This involves a combination of treatment measures, integrating pharmacologic protocols targeting all four mechanisms involved in acne pathogenesis: increased follicular keratinization, increased sebum production, bacterial lipolysis of sebum triglycerides to free fatty acids, and inflammation.
The most critical target for treatment is the microcomedone, as the entire pathogenic cascade of acne is arrested if follicular occlusion is minimized or reversed. This involves a combination of treatment measures, integrating pharmacologic protocols targeting all four mechanisms involved in acne pathogenesis: increased follicular keratinization, increased sebum production, bacterial lipolysis of sebum triglycerides to free fatty acids, and inflammation.
![]() Nondrug measures are aimed at both long-term prevention and treatment. Patients should eliminate aggravating factors, maintain a balanced, low-glycemic load diet, and control stress. They should wash twice daily with a mild soap or soapless cleanser, and restrict cosmetic use to oil-free products. Comedone extraction results in immediate cosmetic improvement in approximately 10% of patients. Shaving should be done as lightly and infrequently as possible, using a sharp blade or electric razor.
Nondrug measures are aimed at both long-term prevention and treatment. Patients should eliminate aggravating factors, maintain a balanced, low-glycemic load diet, and control stress. They should wash twice daily with a mild soap or soapless cleanser, and restrict cosmetic use to oil-free products. Comedone extraction results in immediate cosmetic improvement in approximately 10% of patients. Shaving should be done as lightly and infrequently as possible, using a sharp blade or electric razor.
![]() First-, second-, and third-line therapies should be selected and altered as appropriate for the severity and staging of the clinical presentation.
First-, second-, and third-line therapies should be selected and altered as appropriate for the severity and staging of the clinical presentation.
![]() Treatment is directed at controlling the disorder, not curing it. Regimens should be tapered over time, adjusting to response. The smallest number of agents should be used at the lowest possible dosages to ensure efficacy, safety, avoidance of resistance, and patient adherence.
Treatment is directed at controlling the disorder, not curing it. Regimens should be tapered over time, adjusting to response. The smallest number of agents should be used at the lowest possible dosages to ensure efficacy, safety, avoidance of resistance, and patient adherence.
![]() Once control is achieved, simplify the regimen but continue with some suppressive therapy. It takes 8 weeks for a microcomedone to mature; thus, any therapy must be continued beyond this duration to assess efficacy in terms of comedonal and inflammatory lesion count, control or progression of severity, and management of associated anxiety or depression. Safety end points include monitoring for adverse effects of treatment.
Once control is achieved, simplify the regimen but continue with some suppressive therapy. It takes 8 weeks for a microcomedone to mature; thus, any therapy must be continued beyond this duration to assess efficacy in terms of comedonal and inflammatory lesion count, control or progression of severity, and management of associated anxiety or depression. Safety end points include monitoring for adverse effects of treatment.
![]() Through empathic and informative counseling, the health professional can motivate the patient to continue long-term therapy.
Through empathic and informative counseling, the health professional can motivate the patient to continue long-term therapy.
In this chapter, I review the latest developments in understanding acne vulgaris and its treatment. The contents provide an analysis of the physiology of the pilosebaceous unit; the epidemiology, etiology and pathophysiology of acne; relevant treatment with nondrug measures; and comparisons of pharmacologic agents, including drugs of choice recommended in best-practice guidelines. Options include a variety of alternatives such as retinoids, antimicrobial agents, hormones, and light therapy. Formulation principles are discussed in relation to drug delivery. Patient assessment, general approaches to individualized therapy plans, and monitoring evaluation strategies are presented.
EPIDEMIOLOGY
![]() Acne vulgaris is a chronic disease and the most common one treated by dermatologists. The lifetime prevalence of acne approaches 90%, with the highest incidence in adolescents. Prevalence data available from the European Union, United States, Australia, and New Zealand show that acne affects 80% of individuals between puberty and 30 years of age, depending on the method of lesion counting.1 Other studies have reported acne in 28% to 61% of school children aged 10 to 12 years; 79% to 95% of those 16 to 18 years of age; and even in children aged 4 to 7 years. If mild manifestations were excluded and only moderate or severe manifestations were considered, the frequency in epidemiological studies in Western industrialized countries was still 20% to 35%.2–4
Acne vulgaris is a chronic disease and the most common one treated by dermatologists. The lifetime prevalence of acne approaches 90%, with the highest incidence in adolescents. Prevalence data available from the European Union, United States, Australia, and New Zealand show that acne affects 80% of individuals between puberty and 30 years of age, depending on the method of lesion counting.1 Other studies have reported acne in 28% to 61% of school children aged 10 to 12 years; 79% to 95% of those 16 to 18 years of age; and even in children aged 4 to 7 years. If mild manifestations were excluded and only moderate or severe manifestations were considered, the frequency in epidemiological studies in Western industrialized countries was still 20% to 35%.2–4
The onset of acne vulgaris during puberty occurs at a younger chronologic age in girls than boys. It is triggered in children by the initiation of androgen production by the adrenal glands and gonads, and it usually subsides after the end of growth. However, to some degree, most patients continue to have symptoms into their mid-20s, and there is evidence that the duration of acne may last into middle age for most women, recorded in 54% of women and 40% of men older than 25 years of age.5 In puberty, acne is often more severe in boys in about 15% of cases, which is tenfold greater than in girls. Women often have more severe forms during adulthood. When untreated, acne usually lasts for several years until it spontaneously remits. After the disease has ended, scars and dyspigmentation are not uncommon permanent negative outcomes.
Genetic factors have been recognized; there is a high concordance among identical twins, and there is also a tendency toward severe acne in patients with a positive family history of acne.
There are believed to be no gender differences in acne prevalence, although such differences are often reported and may represent social biases. In urban clinics, there is a clear preponderance of girls seeking treatment. There is also a perception that acne is less prevalent in rural populations. This is supported by the data from Varanasi where 21.35% of boys (13 to 18 years) from rural areas had acne versus 37.5% of those from the urban areas.6
An international group of epidemiologists, community medicine specialists, and anthropologists have questioned whether acne might be predominantly a disease of Western civilization.7 They assert that since acne vulgaris is nearly universal in westernized societies (afflicting 79% to 95% of the adolescent population), one causative factor might be the Western glycemic diet. While this hypothesis is based on the observation that primitive societies subsisting on traditional (low glycemic) diets have no acne, the theory awaits validation and acceptance by the dermatologic community.
ETIOLOGY
![]() Acne is a multifactorial disease. Genetic, racial, hormonal, dietary, and environmental factors have been implicated in its development. Its psychologic impact can be severe.
Acne is a multifactorial disease. Genetic, racial, hormonal, dietary, and environmental factors have been implicated in its development. Its psychologic impact can be severe.
Four major etiologic factors are involved in the development of acne: increased sebum production, due to hormonal influences; alteration in the keratinization process and hyperproliferation of ductal epidermis; bacterial colonization of the duct with Propionibacterium acnes; and production of inflammation with release of inflammatory mediators in acne sites. These are reviewed in the Pathophysiology section later in this chapter.
The role of heredity in acne has not been clearly defined; however, there is a significant tendency toward more serious involvement if one or both parents had severe acne during their youth.
Environmental factors play a major role in determining the severity and extent of acne and may influence the choice of topical treatments. Heat and humidity may induce comedones; pressure or friction caused by protective devices such as helmets, shoulder pads, or pillows, and excessive scrubbing or washing can exacerbate existing acne by causing microcomedones to rupture. Pressure may cause acne lesions to form in patients who do not have acne vulgaris: this variant is called mechanical acne. Hair styles that are low on the forehead or neck may cause excessive sweating and occlusion, exacerbating acne. In most cases acne is worse in winter and improves during the summer, suggesting a salutary effect of sunlight. However, in some cases exposure to sunlight worsens the disease.8
The importance of psychologic factors in this prolonged and capricious condition has been repeatedly stressed. Emotions such as intense anger and stress can exacerbate acne, causing flares or increasing mechanical manipulation. This is probably the result of increased glucocorticoid secretion by the adrenal glands, which appears to potentiate the effects of androgens.9
Dietary influences are the focus of current investigations. In the past, acne was not felt to be influenced by diet, but patients could restrict certain foods they perceived exacerbate acne (chocolate, cola drinks, milk and milk products).10,11 These recommendations, which still persist in some guidelines, are based on one or two poorly designed studies conducted more than 40 years ago. They have largely been discounted by well-designed current studies. A discussion of the issues surrounding dietary influences is elaborated in the Clinical Controversy on Diet box.
Clinical Controversy…
PATHOPHYSIOLOGY
![]() The pathogenesis of acne progresses through the following four major stages:
The pathogenesis of acne progresses through the following four major stages:
1. Increased follicular keratinization
2. Increased sebum production
3. Bacterial lipolysis of sebum triglycerides to free fatty acids
4. Inflammation
Improved understanding of acne development on a molecular level suggests that acne is a disease that involves both innate and adaptive immune systems and inflammatory events.
Acne usually begins in the prepubertal period, when the adrenal glands mature, and progresses as androgen production and sebaceous gland activity increase with gonad development.
As shown in Figure 77–1, acne results from the development of an obstructed sebaceous follicle, called a microcomedone. Sebaceous glands increase their size and activity in response to circulating androgens. Most patients with acne do not overproduce androgens (with some exceptions); instead, they have sebaceous glands that are hyperresponsive to androgens.12 Patients with acne have a significantly greater number of lobules per gland compared with unaffected individuals.
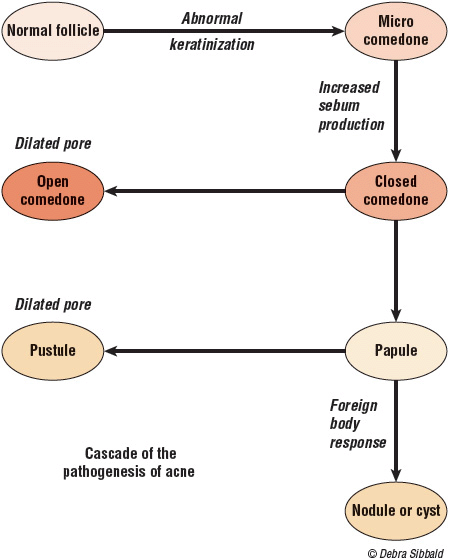
FIGURE 77-1 Cascade of the pathogenesis of acne.
Sebaceous lipids are regulated by peroxisome proliferator-activated receptors, which act in concert with retinoid X receptors to regulate epidermal growth and differentiation as well as lipid metabolism. Sterol response element-binding proteins mediate the increase in sebaceous lipids formation induced by insulin-like growth factor-1. Substance P receptors, neuropeptidases, α-melanocyte stimulating hormone, insulin-like growth factor (IGF)-1R and corticotropin-releasing hormone (CRH)-R1 are also involved in regulating sebocyte activity as are ectopeptidases. The sebaceous gland also acts as an endocrine organ in response to changes in androgens and other hormones. Oxidized squalene can stimulate hyperproliferative behavior of keratinocytes, and lipoperoxides produce leukotriene B4, a powerful chemoattractant.12 The composition of sebum is changed, with a reduction in linoleic acid. The growth of keratinocytes changes. The infrainfundibulum increases its keratinization of cells with hypercornification and development of the microcomedone, the primary lesion of both non-inflammatory and inflammatory acne.13 Cells adhere to each other in an expanding mass, which forms a dense keratinous plug. In particular androgens, hormones could be a stimulus to pilosebaceous duct hypercornification. Sebum, produced in increasing amounts by the active gland, becomes trapped behind the keratin plug and solidifies, contributing to open or closed comedone formation.
Interleukin-1-α upregulation contributes to the development of comedones independently of colonization with Propionibacterium acnes. A relative linoleic acid deficiency has also been described.12
The pooling of sebum in the follicle provides ideal substrate conditions for proliferation of the anaerobic bacterium P. acnes, generating a T cell response, which results in inflammation.13 Propionibacterium acnes produces a lipase that hydrolyzes sebum triglycerides into free fatty acids. These free fatty acids may trigger the changes that lead to an increase in keratinization and microcomedone formation.14,15 This closed comedone, or whitehead, is the first clinically visible lesion of acne. It takes approximately 5 months to develop. The closed comedone is almost completely obstructed to drainage and has a tendency to rupture.16–18
As the plug extends to the upper canal and dilates its opening, an open comedone, or blackhead, is formed. Its dark color is not due to dirt but to either oxidized lipid and melanin or to the impacted mass of horny cells. The cylindrically shaped, open comedone is very stable and may persist for a long time as soluble substances and liquid sebum escape more easily. Acne that is characterized by open and closed comedones is termed noninflammatory acne.
Acne produces chemotactic factors and promotes the synthesis of tumor factor-α and interleukin-1β. Cytokine induction by P. acnes occurs. Both recruitment of polymorphs into the follicle during the inflammatory process and release of P. acnes-generated chemokines lead to pus formation. The pus eventually bursts on the surface with resolution of the inflammation or into the dermis. Propionibacterium acnes also produces enzymes that increase the permeability of the follicular wall, causing it to rupture, releasing keratin, hair, and lipids and irritating free fatty acids into the dermis. Several different types of inflammatory lesions may form, including pustules, nodules, and cysts and may lead to scarring.
Hyperpigmentation and scarring are two sequelae of acne. A time delay of up to 3 years between acne onset and adequate treatment correlates to degree of scarring and emphasizes the need for early therapy.10,11
CLINICAL PRESENTATION AND DIAGNOSTIC CONSIDERATIONS
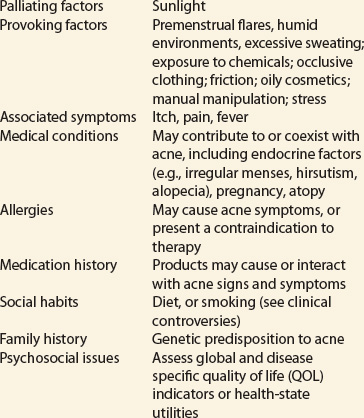
To correctly diagnose acne vulgaris, the clinician considers patient assessment, which includes distinguishing all the presenting signs and symptoms of the clinical presentation, reviewing diagnostic and assessment considerations (see Clinical Presentation box), as well as considering psychosocial issues, differential diagnosis, and the possibility of drug-induced acne.
Psychosocial Issues
Assessment of acne’s impact on quality of life is an important consideration in clinical decision making. The negative impact of facial acne is one of the primary motivators for patients to seek and to adhere to treatment.21 Specific quality of life (QOL) indicators represent patients’ perceptions and reactions to their health. Assessing QOL impairment in patients with acne may aid in management by evaluating psychologic impacts, which may not correlate with clinical severity; aid in detection of depression or need for psychologic care; and improve therapeutic outcomes.
CLINICAL PRESENTATION
Examples of global scales that have been used to evaluate acne include Skindex23 and Dermatology QOL Index;24 examples of acne specific scales include the Acne-specific QOL questionnaire25 and the Acne QOL Scale.26 The Acne QOL Scale was developed to measure the impact of facial acne across four domains (acne symptoms, role-emotional, self-perception, and role-social) of health-related QOL. Health-state utilities (such as time trade-off [TTO]) are quantitative measures of patient preferences of health outcomes ranging from 0 (death) to 1 (perfect health) and can be used in clinical trials as outcome measures of treatment effects. TTO utilities for acne in the range of 0.94 to 0.96 can be compared with those of other diseases (e.g., 0.92 for epilepsy, 0.94 for myopia), and help to identify the impact of acne on self-perception and psychologic functioning.27
Differential Diagnosis
Acne vulgaris is rarely misdiagnosed. The conditions most commonly mistaken for acne vulgaris include rosacea, perioral dermatitis, gram-negative folliculitis, and drug-induced acne.28
Acne rosacea (adult acne) is a chronic relapsing condition, occurring after age 30 years in fair-complexioned persons and involving blood vessels. The first sign is easy flushing followed by development of inflammatory lesions, with edema, papules, and pustules appearing on the nose, cheeks, chin, and forehead, and telangiectasia (spider veins) developing as the condition progresses. The affected area may be sensitive to the touch.
Rosacea (sometimes called adult acne) differs from acne vulgaris in several ways. Its onset is not linked to increased androgens or endocrine changes; comedones are not usually present; aggravating factors are different and include ingestion of alcohol, spicy foods, or hot drinks (especially those containing caffeine); smoking; overexposure to sunlight; and exposure to temperature extremes, friction, irritating cosmetics, and steroids. Rosacea is not curable, progressively worsens, and may ultimately result in rhinophyma (enlarged nose). Refer patients to a physician for treatment, as antibiotics, particularly topical metronidazole, may be required.29
Perioral dermatitis occurs primarily in young women and adolescents and is characterized by erythema, scaling, and papulopustular lesions commonly clustered around the nasolabial folds, mouth, and chin. The cause is unknown.29
Gram-negative folliculitis (Proteus, Pseudomonas, Klebsiella) may complicate acne, with a sudden change to pustules or large inflammatory cysts occurring after long-term treatment of acne with oral antibiotics. Folliculitis may be caused by staphylococci. There is a sudden onset of superficial pustules around the nose, chin, and cheeks. Patients with suspected folliculitis should be referred to a physician.29
Several conditions include acne vulgaris as a characteristic component, and understanding the mechanisms involved in these syndromes provides insight into the pathogenesis of acne. These include polycystic ovary syndrome (elevated androgen levels); PAPA syndrome (pyogenic arthritis, pyoderma gangrenosum, acne; early onset arthritis with increased inflammatory activity), and SAPHO syndrome (synovitis, acne, pustulosis, hyperostosis, osteitis syndrome; sterile inflammatory arthro-osteitis, with P. acnes as a possible trigger).13
Drug-Induced Acne
In addition to the conditions induced by drugs that were presented in eChapter 23, acneiform eruptions can also be caused by medications. Systemic corticosteroids can cause a pustular inflammatory form of acne, especially on the trunk. Onset is abrupt at 2 to 6 weeks after initiation of therapy. Acne has also been associated with most of the potent topical steroids, but not with hydrocortisone, which lacks the ability to inhibit protein synthesis. Discontinuation of the steroid results in an initial worsening of appearance due to removal of the antiinflammatory action of the steroid itself. Caution patients about this reaction, which can be subdued through judicious use of topical hydrocortisone.30–32
Antiepileptics and tuberculostatics are the most commonly implicated in drug-induced acne, followed by lithium. Other heavy metals inducing acne include cobalt in vitamin B12.33 Halogens, especially an excess of iodide in seafood, salt, and health foods, can exacerbate acne. In addition, halogens can provoke de novo acne lesions in individuals who have increased external exposure often due to occupational contact, or pool or hot tub disinfection; this variant is called chloracne.
In addition, certain minor ingredients in cosmetics have been implicated in cosmetic acne, including isopropyl myristate, cocoa butter, and fatty acids.
TREATMENT
The first step in determining a safe and efficacious treatment regimen for acne vulgaris is to establish desired outcomes for the patient, regarding both short- and long-term goals.
Desired Outcomes (Goals of Treatment)
![]() Acne vulgaris is now approached as a chronic disease for purpose of treatment, as it demonstrates the typical characteristics of chronicity: patterns of recurrence or relapse; a prolonged course; manifests as either acute outbreaks or slow onset; and has psychological and social impact. Two principles should be born in mind: this chronic nature warrants early and aggressive treatment, and maintenance therapy is often needed for optimal outcomes.
Acne vulgaris is now approached as a chronic disease for purpose of treatment, as it demonstrates the typical characteristics of chronicity: patterns of recurrence or relapse; a prolonged course; manifests as either acute outbreaks or slow onset; and has psychological and social impact. Two principles should be born in mind: this chronic nature warrants early and aggressive treatment, and maintenance therapy is often needed for optimal outcomes.
Acne requires long-term control, as it cannot be cured. This basic premise needs to be stressed with the patient to establish motivation to adhere to lengthy treatment regimens, which involve both addressing current symptoms and signs and taking preventive measures.
Treatment for acne should aim to reduce both severity (considering objective and subjective grading) and recurrences of skin lesions as well as to improve appearance. A significant percentage change in lesion counts should be noted: most patients empirically validate a margin of 10% to 15% reduction in facial lesion counts as appropriate. Patient global self-assessment of acne improvement is a primary outcome.
Basic goals of treatment include alleviation of symptoms by reducing the number and severity of lesions, slowing the progression of signs and symptoms, limiting the disease duration and recurrence, prevention of long-term disfigurement associated with scarring and hyperpigmentation, and avoidance of psychological suffering.
General Approach to Treatment
![]() The most critical target for treatment is the microcomedone, because by eliminating the follicular occlusion the whole cascade of acne is arrested. This will involve a combination of preventive measures to reduce or eliminate risk and aggravating factors and treatment measures. These should integrate nondrug and pharmacologic protocols aimed at cleansing as well as affecting all four mechanisms involved in acne pathogenesis. Combination therapy to target multiple pathogenic steps is often more effective than single therapy, and may offer secondary advantages of decreasing agent-related side effects and minimizing resistance or tolerance to individual treatments.
The most critical target for treatment is the microcomedone, because by eliminating the follicular occlusion the whole cascade of acne is arrested. This will involve a combination of preventive measures to reduce or eliminate risk and aggravating factors and treatment measures. These should integrate nondrug and pharmacologic protocols aimed at cleansing as well as affecting all four mechanisms involved in acne pathogenesis. Combination therapy to target multiple pathogenic steps is often more effective than single therapy, and may offer secondary advantages of decreasing agent-related side effects and minimizing resistance or tolerance to individual treatments.
The approach to acne management is largely determined by:
1. Severity index
2. Lesion type: predominantly noninflammatory or inflammatory
3. Treatment preferences including patient choices
4. Cost implications
5. Skin type and/or ethnic group
6. Patient age
7. Adherence
8. Response to previous therapy
9. Presence of scarring
10. Psychological effects
11. Family history of persistent acne
Topical therapy is the standard of care for mild-to-moderate acne. Those with moderate-to-severe acne will require systemic therapy.
Topical treatments only work where applied. Because topical therapies reduce new lesion development, they require application to the whole affected area rather than individual spots. Most cause initial skin irritation, and some people stop using them because of this. The irritation can be minimized by starting with lower strength preparations and gradually increasing frequency or dose. Where irritation persists, a change in formulation from alcoholic solutions to washes, gels, or more moisturizing creams or lotions might help.
![]()
![]() First-line, second-line, and third-line therapies should be selected and altered as appropriate for the severity and staging of the clinical presentation. Treatment is directed at controlling the disorder, not curing it. Regimens should be tapered over time, adjusting to response. The smallest number of agents should be used at the lowest possible dosages to ensure efficacy, safety, avoidance of resistance, and patient adherence. Once control is achieved, simplify the regimen but continue with some suppressive therapy. It takes 8 weeks for a microcomedone to mature, thus any therapy must be continued beyond this duration in order to assess efficacy.32 Most topical preparations may be used for years as needed.
First-line, second-line, and third-line therapies should be selected and altered as appropriate for the severity and staging of the clinical presentation. Treatment is directed at controlling the disorder, not curing it. Regimens should be tapered over time, adjusting to response. The smallest number of agents should be used at the lowest possible dosages to ensure efficacy, safety, avoidance of resistance, and patient adherence. Once control is achieved, simplify the regimen but continue with some suppressive therapy. It takes 8 weeks for a microcomedone to mature, thus any therapy must be continued beyond this duration in order to assess efficacy.32 Most topical preparations may be used for years as needed.
Because acne is a chronic disease, lesions typically recur for years. Microcomedones significantly decrease during therapy but rebound almost immediately after therapy is discontinued. Hence, the strategy for treating acne today includes an induction phase followed by a maintenance phase, and is further supported by adjunctive treatments and/or cosmetic routines. A routine part of acne therapy should include maintenance therapy to reduce the potential for recurrence of visible lesions, where maintenance therapy is the regular use of appropriate agents to ensure remission.
For successful long-term treatment, maintenance therapy must be tolerable, appropriate for the patient’s lifestyle and convenient, continuing months to years, depending on age. Education about pathophysiology of acne, and the psychosocial benefits of clearer skin are compelling reasons for patient adherence to consistent therapy to sustain remission.
Nonpharmacologic Therapy
![]()
![]() Encourage patients with acne to discontinue or avoid any aggravating factors, maintain a balanced, low-glycemic-load diet and control stress. Evidence shows that by being empathic and informative during counseling, the health professional may motivate the patient to continue long-term therapy.8,9,28 One of the first approaches to nondrug management of acne is attention to cleansing techniques. Shaving recommendations, comedone extraction, dietary considerations, issues relating to ultraviolet light, and prevention of cosmetic acne should be reviewed with patients.
Encourage patients with acne to discontinue or avoid any aggravating factors, maintain a balanced, low-glycemic-load diet and control stress. Evidence shows that by being empathic and informative during counseling, the health professional may motivate the patient to continue long-term therapy.8,9,28 One of the first approaches to nondrug management of acne is attention to cleansing techniques. Shaving recommendations, comedone extraction, dietary considerations, issues relating to ultraviolet light, and prevention of cosmetic acne should be reviewed with patients.
Cleansing
Cleansers often contain surfactant systems to remove fat from the skin surface. The oil is dispersed from the skin into the surfactant system; however, the active ingredient is sometimes trapped and removed upon rinsing. Also, the balance between cleanliness and drying or irritation should be taken into account. Most patients prefer products with foaming action, and these must contain additional secondary surfactants to enhance the foam and condition the skin.
Soaps are the most widely used cleansing products, but do not lend themselves to efficient delivery of active drug. Two main disadvantages exist. As soaps are rinsed off, the deposit of active agent will be small; and the high pH required in soaps may degrade some active ingredients and be less tolerable on sensitive skin. Soapless cleansers are an alternative to soaps.34
Patients should wash no more than twice daily with a mild, nonfragranced opaque or glycerin soap or a soapless cleanser. Acne patients often wash too frequently, attempting to remove surface oils. There is no evidence indicating that this is helpful, as surface lipids do not affect acne. Contributory lipids are deep in the follicle and are not removed through washing. Antiseptic cleansers, while producing a clean, refreshed feeling, remove only surface dirt, oil, and aerobic bacteria. They do not affect P. acnes. There is no evidence that any particular washing regimen is superior. Evidence-based studies on the use of cleanser or medicated cleansers are lacking or poorly designed with small numbers of patients.35 Scrubbing should be minimized to prevent follicular rupture. Soaps produce a drying effect on the skin due to detergent action. As medicated cleansers require increased contact time, this drying action is pronounced, especially with peeling agents. Avoid cream-based cleansers.
Because the acid pH of skin has an antimicrobial effect, it has been proposed that lowering lesional surface pH (with products such as Herpifix, marketed in Europe) may be correlated to the number of acne lesions. Studies are planned.
Polyester cleansing sponges (e.g., Buf-Puf) are synthetics that abrade the skin surface, removing superficial debris. They are unlikely to unseat comedones, considering the structure of these lesions. The sponges are available in soft or coarse textures, with or without soap. Caution patients against using a circular or rubbing motion that will increase irritation, and instruct them to use single, gentle, continuous strokes on each side of the face, from the midline out toward the ears.
Cationic-bond strips that become activated by water are available. The dirt and oil in the pores is anionic. As the strip dries, the cationic-bond binds the anionic dirt and removes it when the strip is peeled off.
Shaving
Males should try both electric and safety razors to determine which is more comfortable for shaving. When using a safety razor, the beard should be softened with soap and warm water or shaving gel. Shaving should be done as lightly and infrequently as possible, using a sharp blade and being careful to avoid nicking lesions. Strokes should be in the direction of hair growth, shaving each area only once.
Comedone Extraction
Comedone extraction is useful and painless and results in immediate cosmetic improvement although it has not been widely tested in clinical trials. Pretreatment with a peeler for 4 to 6 weeks often facilitates the procedure.32 Following cleansing with hot water, a comedone extractor is placed over the lesion and gentle pressure applied until the contents are expressed. This removes unsightly lesions, preventing progression to inflammation. A correctly sized extractor allows the central keratin plug to extrude through the opening. The small end of a plastic eye dropper, with bulb removed, may also be used. These instruments should be cleaned with alcohol after each use. Some initial reddening may be apparent. If the contents are not expressed with modest pressure, patients should not continue since improper extraction may further irritate the skin. A physician should be consulted if this technique is too difficult for the patient to manage. Since the follicle is difficult to remove completely, comedones may recur between 25 and 50 days following expression. Fewer than 10% of comedone extractions are a complete success, but the process is useful when done properly.19
Comedo removal may be helpful in the management of comedones resistant to other therapies, but it has not been well studied despite long-standing clinical use. Also, while the procedure cannot affect the clinical course of the disease, it can improve the patient’s appearance, which may positively affect adherence with the treatment program.
Ultraviolet Light
Although ultraviolet light was recommended in the past for desquamation, the practice is no longer advisable because of the well-established carcinogenic and photoaging effects of ultraviolet exposure. Moreover, inflamed skin is more susceptible to the damaging effects of ultraviolet light. Patients taking tretinoin may show heightened sensitivity.36
Before exposure to sunlight, patients with acne should apply sunscreens (sun protection factor [SPF] 15) in alcohol or oil-free bases and avoid using the acnegenic benzophenones. Sunscreen should be applied as the first product.
Prevention of Cosmetic Acne
Persistent low-grade acne in women after their mid-20s is frequently caused by heavy cosmetic use. Adolescent acne in younger women may be exacerbated with makeup overuse. The problem is perpetuated when the resultant blemishes are concealed with more cosmetics.
Advise patients to stop using oil-containing cosmetics and avoid cosmetic programs that advocate applying multiple layers of cream-based cleansers and cover-ups. These are advertised through the media and often available through Internet shopping with promotional bonuses. Three-step basic systems usually combine medicated and nonmedicated ingredients, although it may not be apparent by their cosmetic names that therapeutic agents are included. They often start with cleansers, in lotions or creams, which may contain a multitude of unnecessary ingredients, including medicated peelers, oils, fragrances, and preservatives. Often drugs are included in subtherapeutic or low doses, including salicylic acid, sulfur, or benzoyl peroxide. The second step is generally a “toner” or “refresher” which is usually water- or alcohol-based and might contain medicated ingredients such as α-hydroxy acids (e.g., glycolic acid), which are mild comedolytic agents, or even glycerin as a humectant. The final product, often called intensive or repairing solutions, usually contains the lowest strength of peelers such as benzoyl peroxide, sulfur, or salicylic acid; plus potentially sensitizing fragrances and preservatives; or oil-soluble sunscreens that are not identified on the label. Bases may have significant oil content. There may be additional products to supplement as necessary to the base routine of three steps, such as masks or spot treatments. Multiple-step cosmetic programs are often costly, and should be avoided in favor of simple cleansers and more effective single-ingredient peelers at optimal concentrations.
The term noncomedogenic may refer to either water-based vehicles or products that are free of substances known to induce comedones. They are not necessarily oil free. Water-based cosmetics may contain significant amounts of oil in the form of undiluted vegetable oils, lanolin, fatty acid esters (butyl stearate, isopropyl myristate), fatty acids (stearic acid), fatty acid alcohols, cocoa butter, coconut oil, red veterinary petrolatum, and sunscreens containing benzophenones. Water-based products are more likely to contribute to pore blockage than oil-free products.
Oil-free makeups are well-tolerated and lipstick, eye shadow, eyeliner, eyebrow pencils, and loose face powders are relatively innocuous. Heavier, oil-based preparations, particularly moisturizers and hairsprays, clog pores and accelerate comedone formation.37
The patient should restrict cosmetic use to products labeled oil-free rather than water-based, including makeup, moisturizers, or sunscreens. Coverup cosmetics for acne are available in several skin tones and in lotion and cream forms. They often contain peeling agents, antibacterial agents, or hydroquinone. Most contain sulfur. They may be applied as cosmetics two or three times daily, over the entire face or to individual lesions. However, because the spread time of oil-free makeup is decreased, best results are achieved if applied to one-quarter of the face at a time. Topical medication should be applied after gentle cleansing and a foundation lotion may be used sparingly as a concealer.38,39,40
Because the action of most therapeutic acne agents is to dry the skin, the use of moisturizers is counterproductive. Active agents such as α-hydroxy acids (glycolic, lactic, pyruvic, and citric acids) may be present in the cosmetic formulation, since they reduce corneocyte adhesion.41 Patients with acne should be restricted to oil-free α-hydroxy acid products unless absolutely necessary because of treatment with strong drying agents or isotretinoin.
Vehicles
The formulation of an acne vehicle must consider the technical characteristics of maintaining and delivering the drug in an active state together with the need for an elegant product that the patient will enjoy using, so that it is more likely to be applied as required and deliver the full benefit. Physically and chemically, the vehicle will be used with one or more of the following goals: reduce excess oil, control bacteria associated with acne, reduce the effects of hyperkeratinization, and unclog pores. Performance, safety, and stability should be maximized while addressing technical and commercial factors.
Immiscible liquids might be delivered in oil-in-water or water-in-oil emulsions. In addition to having undesirable oil content, these vehicles also contain humectants, thickeners, preservatives, and fragrance, all of which may be problematic.
Solutions are simpler formulations, and there is a trend to use them as the soaking liquid for wipe products made with fibrous cloths. The viability of these kinds of products must take into consideration whether packages are resealable if they contain multiple wipes, and whether the volatility of the solvent will affect storage and availability of the active agent or cause crystallization. Solutions are used mainly with topical antibiotics, which are often dissolved in specific types of alcohol. Although some antibiotics are only soluble in ethyl alcohol, isopropyl alcohol is generally better able to remove oil from the skin surface and is preferred for nonmedicated vehicles. An 8% glycolic acid solution is available for use alone or for incorporation in topical antibiotic preparations. Solutions and washes can be more easily applied to large areas such as the back.42
Nongreasy solutions, gels, lotions, and creams should be selected as bases for topical acne preparations. Gels are very useful as they are totally oil free along with mixtures of water or alcohol. Lotions and creams will contain some oil-phase ingredients. Discourage moisturizers and oil-based products. Lotions are slightly less drying than gels, and creams are more emollient. Many gels contain ethanol or isopropyl alcohol. Propylene glycol is sometimes present in small amounts to add viscosity and lessen the drying effects of strong peeling agents. Gels are drying but may cause a burning irritation in some patients and may prevent certain kinds of cosmetics from adhering to the skin.37 Propylene glycol gels are easy to apply and dry without a visible or sticky film. Nonalcoholic gels may be as effective and less drying than alcoholic solutions. Alcoholic or acetone gels are usually more drying and provide better penetration of the active ingredient.
The percent contribution of vehicle (placebo) toward reported efficacy of reduction of lesions counts of eight commonly prescribed topical preparations at the end of 10 to 12 weeks of daily administration has been evaluated as a mean value of 55% (range 35% to 82%). This demonstrates the great importance of vehicle effects in topical therapy.43 Consider the patient’s skin type and preferences in the choice of vehicle for topical agents. Patients with oily skin often prefer vehicles with higher proportions of alcohol (solutions and gels), while those with dry or sensitive skin prefer nonirritating lotions and creams. Hydrating and emollient products are often recommended to patients using drying treatment therapies, such as isotretinoin, to control adverse effects and improve adherence to treatment. Lotions can be used with any skin type and can be easily spread over hair-bearing skin, but will cause burning or dryness if they contain propylene glycol. Compatibility of vehicles and agents with cosmetics should also be considered.
How to Use Topical Preparations
Topical preparations should not be applied to individual lesions but to the whole area affected by acne to prevent new lesions from developing, using care around the eyelid, mouth, and neck to avoid chafing. Lotions should be applied with a cotton swab once or twice a day after washing or at bedtime if they leave a visible residue.
Psychologic Approaches, Hypnosis, and Biofeedback
The psychologic effects of acne may be profound and the American Academy of Dermatology expert workgroup unanimously concluded that effective acne treatment can improve the emotional outlook of patients.44 There is weak evidence of the possible benefit of biofeedback-assisted relaxation and cognitive imagery.45,46
Dressings
A pilot double-blind, randomized study of 20 patients has shown some benefit of treatment with a hydrocolloid acne dressing when compared with tape dressings for improving mild to moderate inflammatory acne vulgaris. Results showed greater reduction over 3 to 7 days in the overall severity of acne and inflammation, along with greater improvement in redness, oiliness, dark pigmentation, and sebum casual level. Less ultraviolet B light reaches the skin surface with the hydrocolloid dressing in place.47,48
Pharmacologic Therapy
Successful pharmacologic therapy must address one of the four mechanisms involved in the pathogenesis of acne. There are numerous agents available that prove one or more of these actions and are therefore effective (Table 77–2). However, the choice of active pharmacologic therapy depends on severity.
Mechanisms of drug action relating to acne pathogenesis are illustrated in Figure 77–2.
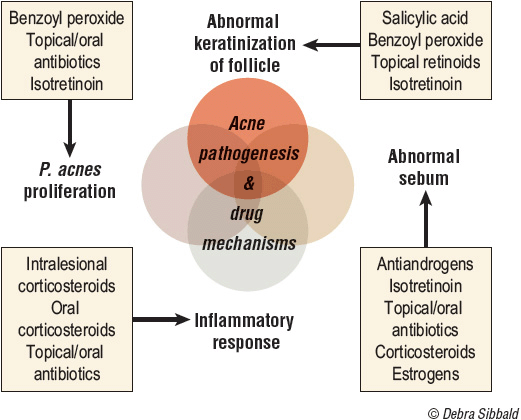
FIGURE 77-2 Acne pathogenesis and drug mechanisms.
Drug Treatments of First Choice
There is concordance among key opinion leaders in different settings regarding recommendations for drugs of choice for management of acne (the Global Alliance,49 European Guidelines12).
For comedonal, noninflammatory acne, active agents of first choice include those that correct the defect in keratinization by producing exfoliation most efficaciously. Topical retinoids, in particular, adapalene, can be recommended as drugs of choice.12,49 Benzoyl peroxide or azelaic acid can be considered, as alternatives (lower strength recommendation)12,49 or a change could be made to an alternate topical retinoid. Limitations can apply that may necessitate the use of a treatment with a lower strength of recommendation as a first-line therapy (e.g., financial resources and reimbursement limitations, legal restrictions, availability, drug licensing). Because the comedone is the initial lesion even in inflammatory acne, these agents are used to correct the defect in keratinization in all cases of acne.
For mild-to-moderate papulopustular inflammatory acne, it is important to reduce the population of P. acnes in the follicle and the generation of its extracellular products and inflammatory effects. Either the fixed-dose combination adapalene and benzoyl peroxide or the fixed-dose combination of clindamycin and benzoyl peroxide are strongly recommended as first choice therapy (high strength recommendation).12,49 As alternatives, a different topical retinoid used with a different topical antimicrobial agent could be advised, with or without benzoyl peroxide. Azelaic acid or benzoyl peroxide can also be recommended (medium strength recommendation). In case of more widespread disease, a combination of a systemic antibiotic with adapalene can be recommended for the treatment of moderate papulopustular acne.
Low-strength recommendations are offered as considerations for treatment in the event of limitations that apply in selecting a first-choice agent. The choices would be blue light monotherapy, fixed-dose combination of erythromycin and tretinoin, fixed-dose combination of isotretinoin and erythromycin, or oral zinc. In case of more widespread disease, a combination of a systemic antibiotic with either benzoyl peroxide or with adapalene in fixed combination with benzoyl peroxide can be considered.12
For severe papulopustular or moderate nodular acne, oral isotretinoin monotherapy is strongly recommended as the drug of first choice (high strength recommendation). As alternatives, medium strength recommendations can be given for systemic antibiotics in combination with adapalene, with the fixed-dose combination of adapalene and benzoyl peroxide or in combination with azelaic acid.12,49 In the event of limitations to use of these agents, considerations could be given to oral antiandrogens in combination with oral antibiotics or topical treatments, or systemic antibiotics in combination with benzoyl peroxide (low strength recommendation).
For nodular or conglobate acne, monotherapy with oral isotretinoin is strongly recommended as the drug of first choice (high strength recommendation).12 As alternative agents, systemic antibiotics in combination with azelaic acid can be recommended (medium strength recommendation). If limitations exist to use of these agents, consideration could be given to oral antiandrogens in combination with oral antibiotics, systemic antibiotics in combination with adapalene, benzoyl peroxide, or the adapalene-benzoyl peroxide fixed-dose combination (low strength recommendation).12
For maintenance therapy for acne, the most recommended agents are topical retinoids. The most extensively studied maintenance treatment (four controlled trials) has been adapalene regimens.12 Other published options include tazarotene or tretinoin. In general, maintenance therapy is begun after a 12-week induction and continues for 3 to 4 months. Continuing improvement using this schema is achieved, with relapse occurring when patients stop treatment, suggesting a longer duration of maintenance therapy is likely to be beneficial. Topical azelaic acid is an alternative to topical retinoids for acne maintenance therapy, with advantageous efficacy and safety profiles for long-term therapy. To minimize antibiotic resistance, long-term therapy with antibiotics is not recommended as an alternative to topical retinoids. If an antimicrobial effect is desired, the addition of benzoyl peroxide to topical retinoid therapy is preferred.
Published Guidelines
In general, recommendations should be based on critical appraisal and interpretation of the literature combined with clinical experience. There is considerable heterogeneity in the acne literature. The large number of products and product combinations, and the scarcity of comparative studies, has led to disparate opinions and few recommendations are evidence-based. Various evidence-based guidelines, available from multiple American, Canadian, European, Scandinavian, and South African sources from 2005 to 2012, do not provide concordance or clarity on all issues.
The 2012 European Guidelines for the Treatment of Acne focus primarily on major treatments, include use of light and laser therapy (see Clinical Controversy on Light Therapy box), but do not review general management issues such as psychological determinants, scarring, diet, and so forth.12 Where relevant, specific information from multiple sources will be integrated into the therapy section that follows.